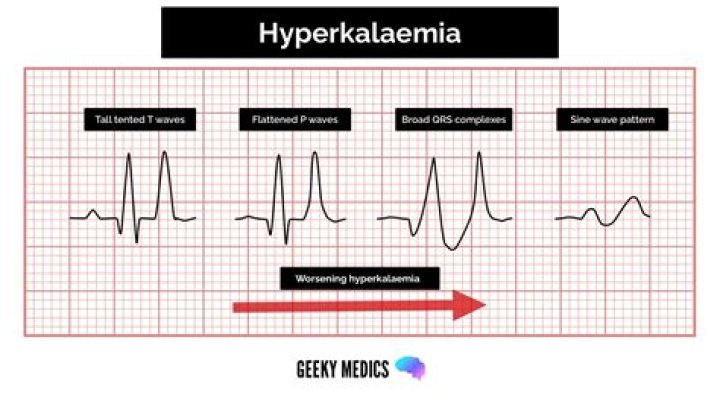
How does Hyperosmolarity cause hyperkalemia

Lily Fisher
Published Apr 24, 2026
Hypertonicity may lead to hyperkalemia by the following 2 mechanisms: Loss of intracellular water, resulting in an increased intracellular potassium concentration, favoring a gradient for potassium to move out of the cells. As water exits the cells, “solvent drag,” which sweeps potassium along.
How does Hyperosmolarity cause hypokalemia?
Hyperosmolarity causes a shift of potassium from within cells to the extracellular space and this potassium is lost as a result of the osmotic diuresis.
What is the major cause of hyperkalemia?
Kidney disease is the most common cause of hyperkalemia. Your kidneys help control the balance of potassium in your body. If they don’t work well, they can’t filter extra potassium from the blood or remove it from the body. A hormone called aldosterone tells the kidneys when to remove potassium.
Why does tissue damage cause hyperkalemia?
The combination of potassium shift out of cells and diminished urine potassium excretion causes hyperkalemia. Another cause of hyperkalemia is tissue destruction, dying cells release potassium into the blood circulation.What are the three causes of hyperkalemia?
- taking in too much potassium.
- potassium shifts due to blood loss or dehydration.
- not being able to excrete potassium through your kidneys properly due to kidney disease.
Does vomiting cause hypokalemia or hyperkalemia?
Vomiting leads to hypokalemia via a complex pathogenesis. Gastric fluid itself contains little potassium, approximately 10 mEq/L. However, vomiting produces volume depletion and metabolic alkalosis, which are accompanied by increased renal potassium excretion.
How do diuretics cause hypokalemia?
Because loop and thiazide diuretics increase sodium delivery to the distal segment of the distal tubule, this increases potassium loss (potentially causing hypokalemia) because the increase in distal tubular sodium concentration stimulates the aldosterone-sensitive sodium pump to increase sodium reabsorption in …
How does hypovolemia cause hyperkalemia?
4.2 Hyperkalemia due to reduced effective plasma volume Reduction in effective plasma volume can occur in hypovolemia but also in hypervolemia, for a variety of reasons including liver or heart failure, third space plasma losses, renal, skin or gastrointestinal fluid losses.Why does hyperkalemia raise resting membrane potential?
Elevated potassium Increased extracellular potassium levels result in depolarization of the membrane potentials of cells due to the increase in the equilibrium potential of potassium. This depolarization opens some voltage-gated sodium channels, but also increases the inactivation at the same time.
Why does hyperkalemia cause excitability?First, in the setting of hyperkalemia, the resting membrane potential is shifted to a less negative value, that is, from −90 mV to −80 mV, which in turn moves the resting membrane potential closer to the normal threshold potential of −75 mV, resulting in increased myocyte excitability.
Article first time published onWhy does hyperkalemia cause metabolic acidosis?
Conclusions Hyperkalemia decreases proximal tubule ammonia generation and collecting duct ammonia transport, leading to impaired ammonia excretion that causes metabolic acidosis.
What is the most common cause of hypokalemia?
Low potassium (hypokalemia) has many causes. The most common cause is excessive potassium loss in urine due to prescription medications that increase urination. Also known as water pills or diuretics, these types of medications are often prescribed for people who have high blood pressure or heart disease.
Why does dehydration cause hyperkalemia?
The body becomes dehydrated when it loses more fluids than it consumes. When the body doesn’t have enough fluids, it can’t process potassium properly, and potassium builds up in the blood, which can lead to hyperkalemia.
Does hyperkalemia cause bleeding?
Hyperkalemia accompanies hemorrhagic shock and, in addition to providing an early sign of the acute ischemic insult severity, may be responsible for cardiac arrest related to hemorrhagic shock.
How does HCTZ cause hypercalcemia?
Hypercalcemia. By increasing calcium reabsorption from the luminal membrane into the interstitium in exchange for sodium, thiazides reduce urine calcium levels and increase blood calcium.
Why do loop diuretics cause hypernatremia?
Renal causes of hypernatremia and volume depletion include therapy with diuretics. Loop diuretics inhibit sodium reabsorption in the concentrating portion of the nephrons and can increase water clearance.
What diuretic causes hyperkalemia?
Hyperkalemia. Potassium-sparing diuretics such as spironolactone, amiloride, and triamterene all have the potential to cause hyperkalemia.
How does vomiting cause hyperkalemia?
Upper gastrointestinal loses –voluminous vomiting causes a rise in bicarbonate concentration due to large losses of gastric acid. This, in conjunction with hypovolemia- induced aldosterone secretion, causes increased potassium secretion and large urinary potassium losses.
How does hypokalemia cause metabolic alkalosis?
Hypokalemia adds to net acid excretion and increases ammoniagenesis perpetuating the severity of metabolic alkalosis. Severe potassium depletion leads to redistribution of H+ from the ECF to ICF. In the process, ECF HCO3– is gained.
Why does hypokalemia cause ventricular tachycardia?
The prolongation of ventricular repolarization in hypokalemic setting is caused by inhibition of outward potassium currents and often associated with increased propensity for early afterdepolarizations. Slowed conduction is attributed to membrane hyperpolarization and increased excitation threshold.
How does hypokalemia affect membrane potential?
The threshold cell membrane potential Hypokalemia increases the resting potential (i.e., makes it more negative) and hyperpolarizes the cell, whereas hyperkalemia decreases the resting potential (i.e., makes it less negative) and initially makes the cell hyperexcitable (Fig. 5-2).
What effect does hypokalemia have on the movement of potassium across the cell membrane why?
Serum hypokalemia causes hyperpolarization of the RMP (the RMP becomes more negative) due to the altered K+ gradient. As a result, a greater than normal stimulus is required for depolarization of the membrane in order to initiate an action potential (the cells become less excitable).
How does hypercalcemia affect resting membrane potential?
High Ca2+ levels can block sodium movement through voltage-gated sodium channels, retarding sodium entry into excitable membranes. Thus, generation of action potentials is altered in neurons as well as skeletal and cardiac muscle cells.
Why do ACE inhibitors cause hyperkalemia?
Main mechanisms contributing to hyperkalemia with ACEi/ARB include decreased aldosterone concentrations, decreased delivery of sodium to the distal nephron, abnormal collecting tubule function, and excessive potassium intake (Table 1).
Can volume depletion cause hyperkalemia?
Hyperkalemia is usually not seen until the glomerular filtration rate falls below 30 ml/min. This is commonly due to primary renal dysfunction but may be due to acute volume depletion from dehydration or bleeding or decreased circulating blood volume due to congestive heart failure or cirrhosis.
How does cirrhosis cause hyperkalemia?
concluded that potassium imbalances are commonly seen in cirrhotic patients, and hyperkalemia is associated with increased serum creatinine and urea levels [7]. Mohsin et al.
How do hypokalemia and hyperkalemia alter the cardiac cell membrane potential and the ability of heart muscle to contract?
Hypokalemia increases the resting potential (i.e., makes it more negative) and hyperpolarizes the cell, whereas hyperkalemia decreases the resting potential (i.e., makes it less negative) and initially makes the cell hyperexcitable (Fig. 5-2).
Why does hyperkalemia cause paralysis?
In hyperkalemic periodic paralysis, high levels of potassium in the blood interact with genetically caused abnormalities in sodium channels (pores that allow the passage of sodium molecules) in muscle cells, resulting in temporary muscle weakness and, when severe, in temporary paralysis.
What would happen to diffusion of potassium and the membrane potential if potassium were decreased in the extracellular fluid?
decrease the membrane potential (depolarize the cell) because the reduction in the equilibrium potential for potassium will mean less potassium will diffuse out of the cell, leaving the interior more positive than before.
Does alkalosis cause hyperkalemia?
Students of laboratory medicine will learn that in general acidemia (reduced blood pH) is associated with increased plasma potassium concentration (hyperkalemia), whilst alkalemia (increased blood pH) is associated with reduced plasma potassium concentration (hypokalemia).
How does potassium affect pH?
Acid-base disturbances cause potassium to shift into and out of cells, a phenomenon called “internal potassium balance” [2]. An often-quoted study found that the plasma potassium concentration will rise by 0.6 mEq/L for every 0.1 unit reduction of the extracellular pH [3].