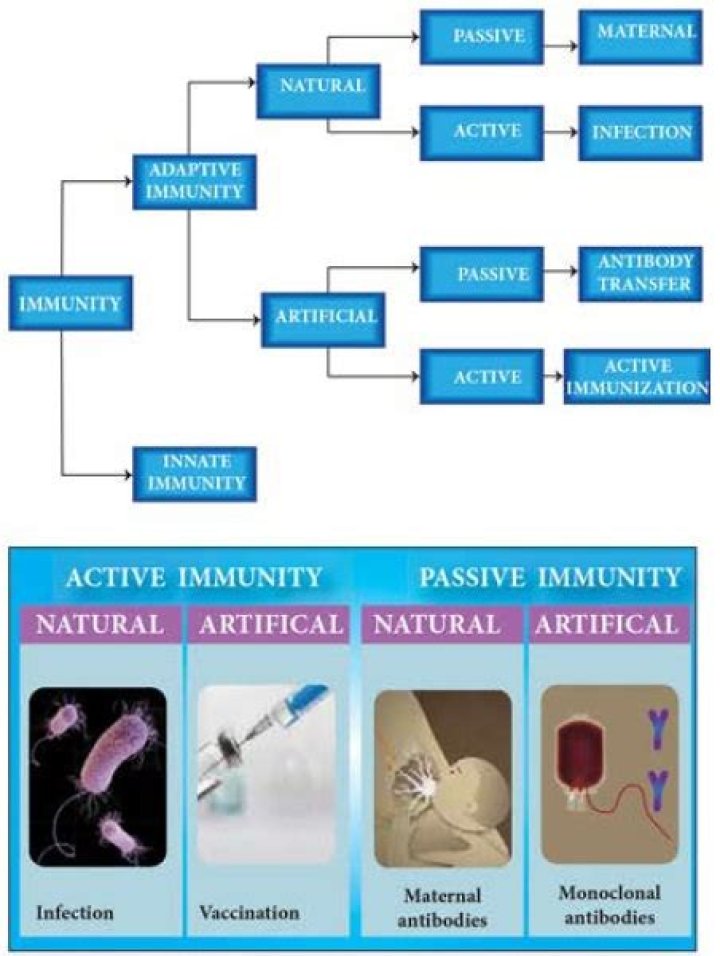
Is active immunity specific or nonspecific

Rachel Hunter
Published Mar 08, 2026
The second line of defense against non-self pathogens is called adaptive immune response. Adaptive immunity is also referred to as acquired immunity or specific immunity and is only found in vertebrates. The adaptive immune response is specific to the pathogen presented.
Is active immunity specific?
Active ImmunityPassive ImmunityProduced by memory cells?YesNo
Is immunity specific or nonspecific?
Immunity from disease is actually conferred by two cooperative defense systems, called nonspecific, innate immunity and specific, acquired immunity. Nonspecific protective mechanisms repel all microorganisms equally, while the specific immune responses are tailored to particular types of invaders.
Is passive immunity specific or nonspecific?
Your immune system builds a defense against that specific antigen. Passive immunity is due to antibodies that are produced in a body other than your own. Infants have passive immunity because they are born with antibodies that are transferred through the placenta from their mother.What is an example of active immunity?
Active immunity can arise naturally, as when someone is exposed to a pathogen. For example, an individual who recovers from a first case of the measles is immune to further infection…
What is meant by active immunization?
From Wikipedia, the free encyclopedia. Active immunization is the induction of immunity after exposure to an antigen. Antibodies are created by the recipient and may be stored permanently.
Is active immunity quick?
Active immunity is quick and gives full response.
What is the key difference between active immunity and passive immunity?
Active immunity occurs when our own immune system is responsible for protecting us from a pathogen. Passive immunity occurs when we are protected from a pathogen by immunity gained from someone else.What is active and passive immunization?
Active immunization is when we give you a vaccine and your immune system kicks into high gear, and sets up a series of reactions in your body to trick your body into thinking that you’ve actually had the disease. Passive immunization is when you get those pre-formed antibodies.
What are examples of passive immunity?Passive immunity can occur naturally, such as when an infant receives a mother’s antibodies through the placenta or breast milk, or artificially, such as when a person receives antibodies in the form of an injection (gamma globulin injection).
Article first time published onWhat is non immunity?
Definition of nonimmune 1 : not produced by, involved in, or relating to an immune response or the immune system nonimmune cells a nonimmune inflammatory response. 2 : lacking immunity (as to a disease) travelers who are nonimmune to local illnesses.
How is active immunity created?
Active Immunity results when exposure to a disease organism triggers the immune system to produce antibodies to that disease. Active immunity can be acquired through natural immunity or vaccine-induced immunity.
Which of the following immunity is non-specific?
Phagocytes are the component of non-specific immune response and kill by engulfing the pathogens that invade the body. They are cells that protect the body by ingesting harmful foreign particles, bacteria, and dead or dying cells.
What are characteristics of active immunity?
In active immunity, the immune cells of the body recognize foreign particles and cells and create antibodies to combat them. Passive immunity, on the other hand, simply gives an organism the correct antibodies to combat germs and pathogens.
Is vaccine passive immunity?
A vaccine may also confer passive immunity by providing antibodies or lymphocytes already made by an animal or human donor. Vaccines are usually administered by injection (parenteral administration), but some are given orally or even nasally (in the case of flu vaccine).
What is active immunity in animals?
Active immunization involves administration of vaccines containing antigenic molecules (or genes for these molecules) derived from infectious agents. In response, the animals mount adaptive immune responses and develop prolonged, strong immunity to those agents.
Why does active immunity last longer?
Active Immunity As long as the memory cells survive, the pathogen will be unable to cause a serious infection in the body. Some memory cells last for a lifetime and confer permanent immunity. Active immunity can also result from immunization.
When are readymade antibodies directly given?
When ready-made antibodies are directly given, it is called Passive immunity.
What is natural active acquired immunity and give an example?
Active immunity is usually classified as natural or acquired. Wild infection for example with hepatitis A virus (HAV) and subsequent recovery gives rise to a natural active immune response usually leading to lifelong protection.
What vaccines are active?
The live, attenuated viral vaccines currently available and routinely recommended in the United States are MMR, varicella, rotavirus, and influenza (intranasal). Other non-routinely recommended live vaccines include adenovirus vaccine (used by the military), typhoid vaccine (Ty21a), and Bacille Calmette-Guerin (BCG).
Which of the following is an active form of immunization?
The 2 major approaches to active immunization are (1) live, attenuated vaccines and (2) inactivated or detoxified agents or their purified components. For some diseases, such as poliomyelitis and influenza, both approaches have been used.
Is toxoid active or passive immunity?
Tetanus toxoids are antigens used as a vaccine for tetanus which promotes antibody formation in body and provide Artificial active immunity…
What is different between active and passive transport?
In Active transport the molecules are moved across the cell membrane, pumping the molecules against the concentration gradient using ATP (energy). In Passive transport, the molecules are moved within and across the cell membrane and thus transporting it through the concentration gradient, without using ATP (energy).
Can you be naturally immune to Covid?
A study from the CDC in September 2021 showed that roughly one-third of those with COVID-19 cases in the study had no apparent natural immunity.
What is the difference between active immunity and passive immunity quizlet?
What is the key difference between active immunity and passive immunity? In active immunity, a body produces its own antibodies; in passive immunity, a person receives pre-made antibodies.
What are the two types of passive immunity?
There are two types of passive immunity: artificial and natural. Artificial passive immunity is achieved by infusion of serum or plasma containing high concentrations of antibody.
What is meant by specific immunity?
Specific immunity, also known as adaptive immunity, is specialized immunity for particular pathogens. Helper T-cells, cytotoxic T-cells, and B-cells are involved in specific immunity. The non-specific cells, like macrophages, tell the T- and B-cells that an intruder is present.
Are granulocytes specific or nonspecific?
Granulocytes are part of the innate immune system, and they have somewhat nonspecific, broad-based activity. They do not respond exclusively to specific antigens, as do B-cells and T-cells.
What are 4 types of immunity?
- Innate immunity: Everyone is born with innate (or natural) immunity, a type of general protection. …
- Adaptive immunity: Adaptive (or active) immunity develops throughout our lives. …
- Passive immunity: Passive immunity is “borrowed” from another source and it lasts for a short time.
What is artificially acquired active immunity?
Artificially acquired active immunity is protection produced by intentional exposure of a person to antigens in a vaccine, so as to produce an active and lasting immune response.
What is a non specific antibody?
Non-specific antibody binding occurs when an antibody binds to a cell that does not have an epitope specifically for that antibody. There are several reasons for non-specific antibody binding. The most common cause is an excess of antibody.



