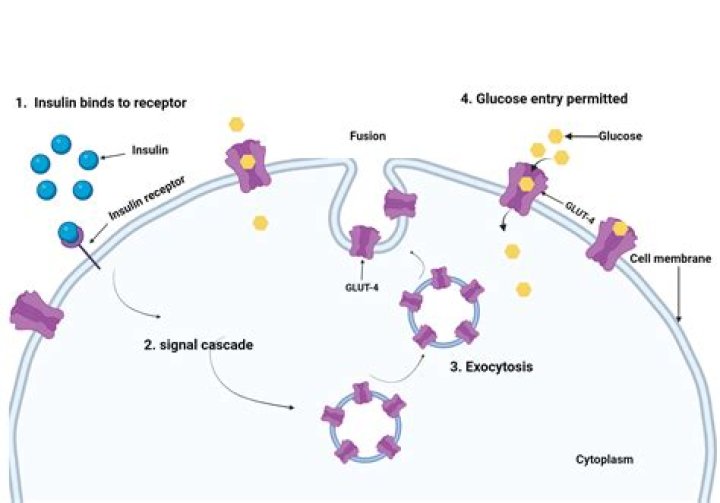
What activates glut4

Isabella Wilson
Published May 12, 2026
The mechanism for GLUT4 is an example of a cascade effect, where binding of a ligand to a membrane receptor amplifies the signal and causes a cellular response. In this case, insulin binds to the insulin receptor in its dimeric form and activates the receptor’s tyrosine-kinase domain.
What increases GLUT4 expression?
Our results show that a rapid increase in GLUT4 expression is an early adaptive response of muscle to exercise. This adaptation appears to be mediated by pretranslational mechanisms. We hypothesize that the physiological role of this adaptation is to enhance replenishment of muscle glycogen stores.
Does insulin activate GLUT4?
Insulin stimulates the translocation of a pool of Glut4 to the plasma membrane, through a process of targeted exocytosis.
How is GLUT4 regulated?
Recent information indicates that glut4 gene transcription is regulated by a number of factors in skeletal muscle that include MEF2, MyoD myogenic proteins, thyroid hormone receptors, Kruppel-like factor KLF15, NF1, Olf-1/Early B cell factor and GEF/HDBP1.What causes translocation of GLUT4?
GLUT4 is present in vesicles in cytoplasm of the cells. Binding of insulin to insulin receptor causes translocation of GLUT4 to cell membrane. GLUT4 vesicles in the skeletal muscle are either transferrin positive or negative and are translocated by different stimuli.
What happens to GLUT4 without insulin?
In resting muscle and adipose cells (i.e., in the absence of insulin), GLUT4 is found in GLUT4 storage vesicles (GSVs) within these cells, with less than 5% of the transporter present on the cell membranes. … The GSVs can be isolated from cells and are found to contain numerous proteins in addition to GLUT4.
How does insulin affect GLUT4?
Insulin increases the steady state plasma membrane levels of GLUT4 5- to 30-fold.
Does insulin promote fat breakdown?
Insulin plays a role in regulating blood sugar levels and converting food energy into fat. It also helps break down fats and proteins. During digestion, insulin stimulates muscle, fat, and liver cells to absorb glucose. The cells either use this glucose for energy or convert it into fat for long-term storage.Does insulin stimulate glycogen breakdown?
Glycogen breakdown is stimulated not only by the absense of insulin but by the presence of glucagon, which is secreted when blood glucose levels fall below the normal range.
What path does insulin activate?The insulin transduction pathway is a biochemical pathway by which insulin increases the uptake of glucose into fat and muscle cells and reduces the synthesis of glucose in the liver and hence is involved in maintaining glucose homeostasis.
Article first time published onWhat is the function of protein GLUT4?
Skeletal muscle both stores glucose as glycogen and oxidizes it to produce energy following the transport step. The principal glucose transporter protein that mediates this uptake is GLUT4, which plays a key role in regulating whole body glucose homeostasis.
Does GLUT4 use ATP?
GLUT4 is one of 13 sugar transporter proteins (GLUT1-GLUT12, and HMIT) encoded in the human genome (Joost and Thorens, 2001, Wood and Trayhurn, 2003) that catalyzes hexose transport across cell membranes through an ATP-independent, facilitative diffusion mechanism (Hruz and Mueckler, 2001).
Does GLUT4 require ATP?
These data suggest that GLUT4 recycles from the cell surface both in the presence and absence of insulin. … We conclude that the insulin-stimulated movement of GLUT4 to the cell surface in adipocytes may require ATP early in the insulin signaling pathway and a GTP-binding protein(s) at a later step(s).
Is GLUT4 bidirectional?
Class I comprises the well-characterized glucose transporters GLUT1-GLUT4. Is widely distributed in fetal tissues. … Is a bidirectional transporter, allowing glucose to flow in 2 directions. Is expressed by renal tubular cells, liver cells and pancreatic beta cells.
What is glut biochemistry?
Glucose transporter (GLUT) is a facilitative transport protein involved in glucose translocation across the cell membrane.
How does exercise increase glucose uptake?
The increase in skeletal muscle glucose uptake during exercise results from a coordinated increase in rates of glucose delivery (higher capillary perfusion), surface membrane glucose transport, and intracellular substrate flux through glycolysis.
What happens when GLUT4 is damaged?
Translocation is the process by which vesicles in the cytoplasm containing GLUT4 move to the plasma membrane and fuse with it under the stimulation of insulin. Malfunction of the process can lead to insulin resistance (Peck et al., 2009).
Does insulin inhibit gluconeogenesis?
Insulin is a key hormone that inhibits gluconeogenesis, and insulin resistance is a hallmark of type 2 diabetes. Understanding the regulation of gluconeogenesis and the role of insulin signaling in this pathway is important to developing new therapies for type 2 diabetes.
Does liver have GLUT4?
An auxiliary function of some GLUTs in the liver seems to be the transport of dehydroascorbic acid (DHA), the oxidized form of ascorbic acid (AA, vitamin C) as described for the GLUT isoforms GLUT1, GLUT3, and GLUT4 [188].
What happens to glucose when there is no insulin?
Without enough insulin, glucose builds up in the bloodstream instead of going into the cells. This buildup of glucose in the blood is called hyperglycemia.
How is GLUT4 similar to GLUT 1 How are they different?
GLUT1 is expressed in most cells, is localized primarily at the cell membrane, and is thought to participate mainly in basal glucose transport in muscle. GLUT4 is expressed only by cells that accelerate glucose transport in response to insulin (skeletal muscle, heart muscle, and adipose cells).
What stimulates glycogen synthesis?
The insulin hormone stimulates the synthesis of glycogen. When the blood glucose level rises, insulin stimulates glycogen synthase to form glycogen from glucose.
How does insulin activate glycogen synthesis?
Insulin promotes dephosphorylation and activation of glycogen synthase (GS) by inactivating glycogen synthase kinase (GSK) 3 through phosphorylation. Insulin also promotes glucose uptake and glucose 6-phosphate (G-6-P) production, which allosterically activates GS.
Does glucagon stimulate gluconeogenesis?
Here we show that glucagon stimulates hepatic gluconeogenesis by increasing the activity of hepatic adipose triglyceride lipase, intrahepatic lipolysis, hepatic acetyl-CoA content and pyruvate carboxylase flux, while also increasing mitochondrial fat oxidation-all of which are mediated by stimulation of the inositol …
Why do diabetics have large abdomens?
When we drink beverages sweetened with sucrose, fructose, or high fructose corn syrup, the liver stores this extra sugar as fat, increasing belly fat, Norwood says. The hormones produced by this extra belly fat play a role in insulin resistance, possibly leading to type 2 diabetes.
What is a diabetic belly?
Diabetic gastroparesis refers to cases of the digestive condition gastroparesis that diabetes causes. During normal digestion, the stomach contracts to help break down food and move it into the small intestine. Gastroparesis disrupts the stomach’s contraction, which can interrupt digestion.
Why do people with undiagnosed diabetes go to the toilet a lot and are thirsty?
Excessive thirst and increased urination Your kidneys are forced to work overtime to filter and absorb the excess glucose. When your kidneys can’t keep up, the excess glucose is excreted into your urine, dragging along fluids from your tissues, which makes you dehydrated. This will usually leave you feeling thirsty.
Does insulin activate glycogen phosphorylase?
Insulin promotes dephosphorylation and activation of glycogen synthase (GS) by inactivating glycogen synthase kinase (GSK) 3 through phosphorylation. … Basal and epinephrine-stimulated activity of muscle glycogen phosphorylase was comparable between wild-type and GSK3 knockin mice.
What is the insulin signaling cascade?
The insulin signaling pathway is the sum of all proteins involved in the action of insulin in the body and the factors that regulate this pathway. … Fat and protein metabolism is especially prominent, but its physiological function depends on a variety of target tissues and signal transduction pathways within cells.
How is insulin transported?
Transport of circulating insulin from the blood into the central nervous system. (1) Circulating insulin, released into the blood pancreatic β cells, binds to transporters on endothelial cells of the blood–brain barrier. (2) Insulin is transported through endothelial cells by receptor-mediated transcytosis.
Why does GLUT4 need insulin?
Key Points. The glucose transporter GLUT4 facilitates insulin-stimulated glucose uptake into muscle and adipose tissue. … Stimulation with insulin results in regulated exocytosis of GSVs. GSV mobilization, targeting and fusion at the plasma membrane requires coordinated control of the trafficking machinery by insulin.



