What are the three major components of E M documentation Why are there two sets of guidelines 1995 and 1997 and where do they differ in documentation

Dylan Hughes
Published May 15, 2026
The three key components when selecting the appropriate level of E/M services provided are history, examination, and medical decision making.
What are the three major components of EM documentation?
The three key components when selecting the appropriate level of E/M services provided are history, examination, and medical decision making.
What are the guidelines for documentation?
- Stay Up-to-Date. No matter how knowledgeable you are, everyone can use a refresher even in their expert fields. …
- Leverage Strong Tools. …
- Don’t Get Caught Up on Templates. …
- Include Visuals. …
- Set a Time for Writing. …
- Have a Purpose. …
- Keep It Simple.
What are the 3 key elements of medical decision making?
We can call these three elements diagnoses and management options, data and risk. The guidelines follow CPT in recognizing four levels of each of these elements, and four corresponding levels of medical decision making overall (see “The elements of medical decision making”).What is the difference between 1995 and 1997 guidelines?
™ 1995 documentation guidelines – Should describe four or more elements of the present HPI or associated comorbidities. ™ 1997 documentation guidelines – Should describe at least four elements of the present HPI or the status of at least three chronic or inactive conditions.
What are the components of HPI?
- Location. What is the site of the problem? …
- Quality. What is the nature of the pain? …
- Severity. …
- Duration. …
- Timing. …
- Context. …
- Modifying factors. …
- Associated signs and symptoms.
What are the 3 contributing factors that determine the level of EM Service?
The first three of these components (History, Examination, Medical Decision Making) are considered the “key” components in selecting a level of E&M service. The extent of these services are major factors in defining the level of the service performed.
What is a Level 3 physical exam?
A level-III exam is expanded problem-focused, which requires the description of one component of the affected body area or organ system and at least one other affected body area or organ system.What are the 3 major questions coders should ask when identifying an e M code?
These factors — history, exam, and MDM (HEM) — are known as the three key components of E/M level selection. Determining the correct type of history, exam, and MDM can feel intimidating even for seasoned coders because of the many requirements involved.
What are the documentation guidelines for medical services?- Reason for encounter, relevant history, findings, test results and service.
- Assessment and impression of diagnosis.
- Plan of care with date and legible identity of observer.
How many key components of documentation are there?
The E/M key components can be thought of as the building blocks of documentation for all patient encounters. Some types of encounters require complete documentation of all three key components, while others require only two out of three.
What is the purpose of guidelines?
A guideline aims to streamline particular processes according to a set routine or sound practice. Guidelines may be issued by and used by any organization (governmental or private) to make the actions of its employees or divisions more predictable, and presumably of higher quality. A guideline is similar to a rule.
What are guidelines used for?
What is a guideline? Guidelines guide employees through a process or a task. They give general recommendations of how to perform a task, or advice on how to proceed in a situation. They usually provide a good overview of how to act in a situation where there’s no specific policy or standard.
What is the most significant difference between the 1995 and 1997 E M guidelines?
Unlike the 1995 rules, the 1997 version allows physicans to document an extended HPI by commenting on the status of three or more chronic or inactive problems. On the other hand, the 1995 rules state that the physician must use the so-called elements of HPI when completing the history.
What are the elements of the history of present illness according to the 1995 and 1997 documentation guidelines?
HISTORY OF PRESENT ILLNESS (HPI) It includes the following elements: location; quality; severity; duration; timing; context; modifying factors; and associated signs and symptoms.
What is 1995 coding guidelines?
The 1995 documentation guidelines state that the medical record for a general multi-system examination should include findings about eight or more organ systems. The 1995 E/M guidelines should describe four or more elements of the present HPI or associated comorbidities.
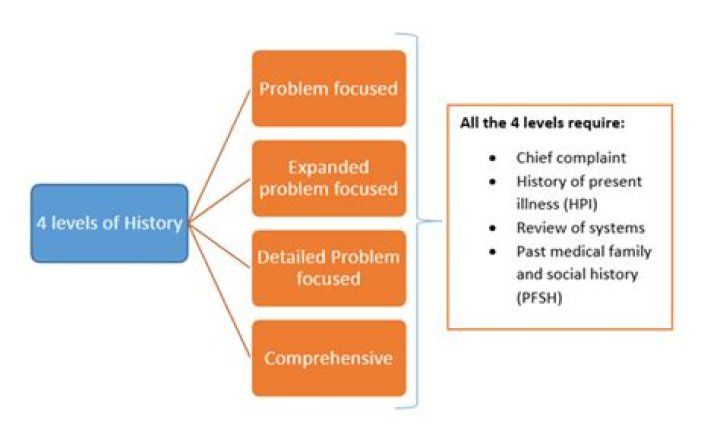
What are the four contributory components of E m?
These components are: History; ▪ Examination; and ▪ Medical Decision Making. A chief complaint is a concise statement summarizing the symptom, problem, condition, diagnosis or reason for the patient encounter. Usually stated in the patient’s own words.
When choosing an em code and all three key components are not met do you select the lower level or higher level?
You must choose your code based on the lowest documented component because you have to meet (or exceed) the requirements for all three components.
How many key components are there when evaluating an e m code quizlet?
The three key components (history, examination, and medical decision making) are required for most E/M codes.
Which are the components of a patient's past health history Select all that apply?
Select all that apply. A patient’s past health history should include past operations, immunizations, hospitalizations, and chronic illnesses.
When the physician determines the patient's main reason for the encounter this information is referred to as the?
When the physician determines the patient’s main reason for the encounter, this information is referred to as the: chief complaint. The modifier -32 is used to indicate: mandated services (used when requested by the payer).
What does HPI mean?
Abbreviation for history of present illness.
What are the key components to be checked when performing a coding audit?
- Are the codes appropriate to the patient’s profile (age, gender, condition; new or established), and is each coded service billable?
- Is there a clear and correct link between each diagnosis and procedure?
What are the key components of the office and other outpatient evaluation and management coding select all that apply?
Office or other outpatient visit for the evaluation and management of a new patient, which requires these 3 key components: A detailed history; A detailed examination; Medical decision making of low complexity.
Which of the following is a component of an E&M code?
E&M services contain three “key” components, history, examination and medical decision making, which are used as a basis for selecting a level of E&M service. Each of these three components have different levels of complexity.
What is a Level 2 E M service?
Level 2 Established Office Visit (99212) This is the second lowest level of care for an established patient being seen in the office. Internists used this code for 2.04% of these encounter in 2019. The Medicare allowable reimbursement for this code is $56.88 and it is worth 0.7 work RVUs.
What is a Level 2 Physical?
Level 2-Cognitive Evaluation (CE) measures your clinical skills and problem-solving techniques over the course of a day-long computerized exam. Level 2-Performance Evaluation (PE) tests your clinical examination skills through physical examinations you’ll conduct on standardized patients.
What is a level 2 physical exam?
Examination Description The COMLEX-USA Level 2-Performance Evaluation (Level 2-PE) is a patient-presentation-based assessment of fundamental clinical skills evaluated through 12 encounters with standardized patients. Candidates assess problem-centered patient presentations.
Why is documentation so important in healthcare?
Good documentation is important to protect your patients. Good documentation promotes patient safety and quality of care. Complete and accurate medical recordkeeping can help ensure that your patients get the right care at the right time. … That is billing when the medical record cannot back up the claim.
What is the purpose of documentation in a patient's medical record?
Clear and concise medical record documentation is critical to providing patients with quality care, ensuring accurate and timely payment for the services furnished, mitigating malpractice risks, and helping healthcare providers evaluate and plan the patient’s treatment and maintain the continuum of care.
What is record documentation?
Records are historical files that provide “proof of existence.” They are used to prove a state of existence of the business. It is either created or received by an organization in connection with business transactions or it can be used for compliance with legal requirements. … In short it is a historical document.