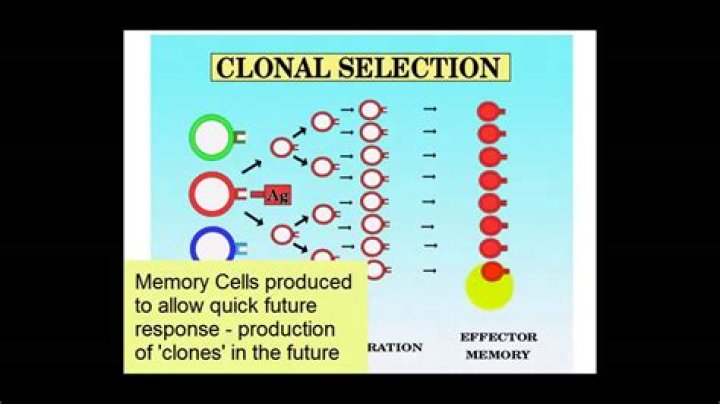
What causes clonal selection

Andrew Campbell
Published Apr 04, 2026
When an antigen encounters the immune system, its epitopes eventually will react only with B-lymphocytes with B-cell receptors on their surface that more or less fit and this activates those B-lymphocytes. This process is known as clonal selection (Figure 13.1E. 2).
What triggers clonal selection?
Clonal selection: The theory that lymphocytes bear antigen receptors before activation and that random mutations during clonal expansion cause the development of lymphocytes with high binding affinities for their antigens. humoral: Of or relating to the body fluids or humors.
What is clonal selection quizlet?
clonal selection. –antigenic-specific selection of a lymphocyte that activates it to produce clones of effector cells dedicated to eliminating the antigen that provoked the initial immune response. – one clone of cells consists of effector cells, another clone of cells consists of memory cells.
What is being selected in clonal selection?
The clonal selection theory proposes that antigen selects lymphocytes for activation from a population of cells precommitted to produce specific antibody. Implicit in this theory is that antibody-forming cells are monospecific and express cell-surface receptors capable of binding foreign antigens.What is clonal selection biology?
Key Terms. clonal selection: An hypothesis which states that an individual lymphocyte (specifically, a B cell) expresses receptors specific to the distinct antigen, determined before the antibody ever encounters the antigen. Binding of Ag to a cell activates the cell, causing a proliferation of clone daughter cells.
Is clonal anergy reversible?
Clonal anergy is another mechanism of peripheral tolerance to self-antigens. In the context of oral tolerance, its involvement was first demonstrated based on a study that showed T cell tolerance could be reversed in vitro by exogenous IL-2 (Whitacre et al., 1991).
What cell releases interferon?
Type I interferon (IFN-alpha and IFN-beta) is secreted by virus-infected cells while type II, immune or gamma interferon (IFN-gamma) is mainly secreted by T cells, natural killer (NK) cells and macrophages.
Which lymphocyte type produces antibodies?
A lymphocyte is a type of white blood cell that is part of the immune system. There are two main types of lymphocytes: B cells and T cells. The B cells produce antibodies that are used to attack invading bacteria, viruses, and toxins.What are the 4 principles of clonal selection theory?
Clonal selection theory of lymphocytes: 1) A hematopoietic stem cell undergoes differentiation and genetic rearrangement to produce 2) immature lymphocytes with many different antigen receptors. Those that bind to 3) antigens from the body’s own tissues are destroyed, while the rest mature into 4) inactive lymphocytes.
Where is adaptive immune initiated?The induction of an adaptive immune response begins when a pathogen is ingested by an immature dendritic cell in the infected tissue. These specialized phagocytic cells are resident in most tissues and are relatively long-lived, turning over at a slow rate.
Article first time published onWhat causes clonal selection quizlet?
Clonal selection occurs when antigen is encountered by: T-cells: Both T-cells and B-cells possess antigen-specific receptors and clones of these lymphocytes will be selected to proliferative when specific antigen is encountered.
What is the purpose of clonal deletion?
Clonal deletion is the removal through apoptosis of B cells and T cells that have expressed receptors for self before developing into fully immunocompetent lymphocytes. This prevents recognition and destruction of self host cells, making it a type of negative selection or central tolerance.
Which of the following is an example of a mechanical barrier to infection?
Mechanical barriers — which include the skin , mucous membranes , and fluids such as tears and urine — physically block pathogens from entering the body.
What triggers interferon production?
Interferon is secreted by cells in response to stimulation by a virus or other foreign substance, but it does not directly inhibit the virus’s multiplication. Rather, it stimulates the infected cells and those nearby to produce proteins that prevent the virus from replicating within them.
How is interferon made?
Interferons are formed when most cells are treated with viruses or double-stranded RNA (to form IFN-alpha or beta, or both) or when lymphoid cells are treated with mitogens or the appropriate antigen (to form IFN-gamma).
Do interferons cause inflammation?
Interferons (IFNs) and pro- and anti-inflammatory cytokines are crucial for appropriate response to pathogens, damaged cells, or irritants in inflammatory response. The inflammasom is multiprotein complex, which initiates cleavage of pro-inflammatory cytokines IL-1β and IL-18 into active forms.
What causes T anergy?
T-cell anergy can arise when the T-cell does not receive appropriate co-stimulation in the presence of specific antigen recognition.
When does clonal anergy occur?
In contrast to low antigen dose T cell clonal anergy, which occurs in the absence of costimulation, T cell anergy induced by human T cell presentation of antigen results in both primary proliferation and secondary unresponsiveness to high-dose antigenic stimulation.
Where does affinity maturation occur?
Affinity maturation primarily occurs on surface immunoglobulin of germinal center B cells and as a direct result of somatic hypermutation (SHM) and selection by TFH cells.
How does a macrophage destroy a pathogen?
When a macrophage ingests a pathogen, the pathogen becomes trapped in a phagosome, which then fuses with a lysosome. Within the phagolysosome, enzymes and toxic peroxides digest the pathogen. However, some bacteria, such as Mycobacterium tuberculosis, have become resistant to these methods of digestion.
Which lymphocyte matures in thymus?
Precursors of T cells migrate from the bone marrow and mature in the thymus. This process is similar to that for B cells, including the sequential rearrangement of antigen receptor gene segments.
What causes increase in lymphocytes?
If your doctor determines that your lymphocyte count is high, the test result might be evidence of one of the following conditions: Infection (bacterial, viral, other) Cancer of the blood or lymphatic system. An autoimmune disorder causing ongoing (chronic) inflammation.
How do lymphocytes develop?
All lymphocytes originate from a common lymphoid progenitor cell known as a lymphoblast, before differentiating into their distinct lymphocyte types. The formation of lymphocytes is known as lymphopoiesis. B cells mature into B lymphocytes in the bone marrow, while T cells migrate to and mature in thymus.
How are lymphocytes produced?
Lymphocytes. White blood cells known as lymphocytes arise from by mitosis of stem cells in the bone marrow. Some lymphocytes migrate to the thymus and become T cells that circulate in the blood and are associated with the lymph nodes and spleen.
What causes an adaptive immune response?
Unlike the innate immune system, which attacks only based on the identification of general threats, the adaptive immunity is activated by exposure to pathogens, and uses an immunological memory to learn about the threat and enhance the immune response accordingly.
What activates the adaptive immune system?
To achieve functional adaptive immune responses, antigen-specific T cell populations are stimulated by professional antigen-presenting cells like dendritic cells (DCs), which provide crucial stimulatory signals for efficient expansion and development of effector functions.
How is innate immunity activated?
The innate immune system is always general, or nonspecific, meaning anything that is identified as foreign or non-self is a target for the innate immune response. The innate immune system is activated by the presence of antigens and their chemical properties.
What does a plasma cell secrete?
Plasma cells are differentiated B-lymphocyte white blood cells capable of secreting immunoglobulin, or antibody. These cells play a significant role in the adaptive immune response, namely, being the main cells responsible for humoral immunity.
What is the major factor regulating the adaptive immune response?
Chapter 10, Question 1. 1 A major factor regulating the adaptive immune response is: A The neutrophil.
Where is IgA secreted?
Secretory IgA Polymeric IgA (mainly the secretory dimer) is produced by plasma cells in the lamina propria adjacent to mucosal surfaces. It binds to the pIgR on the basolateral surface of epithelial cells, and is taken up into the cell via endocytosis.
Which of the following cytokines helps regulate inflammation?
Major anti-inflammatory cytokines include interleukin (IL)-1 receptor antagonist, IL-4, IL-10, IL-11, and IL-13. Leukemia inhibitory factor, interferon-alpha, IL-6, and transforming growth factor (TGF)-β are categorized as either anti-inflammatory or pro-inflammatory cytokines, under various circumstances.



