What is Endo anatomy

Olivia Owen
Published Mar 26, 2026
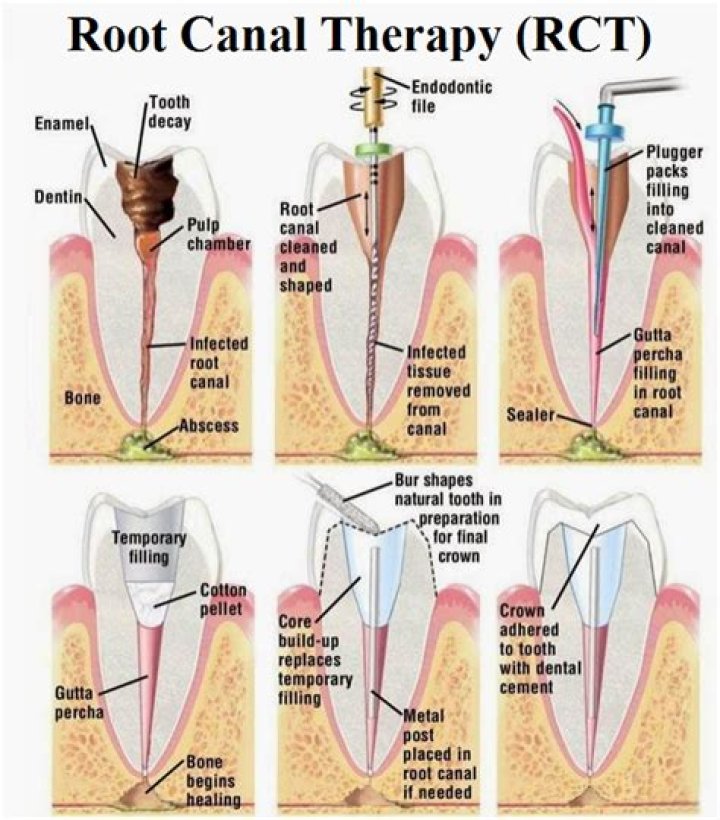
“Endo” is the Greek word for “inside” and “odont” is Greek for “tooth.” Endodontic treatment treats the inside of the tooth. To understand endodontic treatment, it helps to know something about the anatomy of the tooth.
What is Endo infection?
Endodontic infections are polymicrobial and are made up of predominantly anaerobic bacteria and some facultative bacteria. A tooth with an infected nonvital pulp is a reservoir of infection that is isolated from the patient’s immune response and will eventually produce a periradicular inflammatory response.
What is an endo exam?
Membership in Endodontics (M Endo) The examination is a summative assessment of core knowledge and clinical judgement in Endodontics as defined in the Learning Outcomes, and intended to test the candidate’s application of knowledge and clinical judgement at a level expected of a specialist practitioner.
What is Endo fill?
The standard filling material is gutta-percha, a natural polymer prepared from latex from the percha tree (Palaquium gutta). The standard endodontic technique involves inserting a gutta-percha cone (a “point”) into the cleaned-out root canal along with a sealing cement.What is endodontic SAP?
Symptomatic Apical Periodontitis (SAP)– This occurs when infection has caused inflammation of tissue within the pulpal area of the tooth, as well as the tooth’s root canal system AND the periapical tissues.
Who invented root canal?
In 1838, the first root canal therapy tool was invented by American Edwin Maynard, who created it using a watch spring. In 1847, a filling material called gutta percha was first used to fill root canals, a method still practiced to this day.
What is apical periodontitis?
Apical periodontitis is a chronic inflammatory disorder of periradicular tissues caused by aetiological agents of endodontic origin. Persistent apical periodontitis occurs when root canal treatment of apical periodontitis has not adequately eliminated intraradicular infection.
What is root canal and crown?
A root canal is performed when the endodontist removes the infected pulp and nerve in the root of the tooth, cleans and shapes the inside of the root canal, then fills and seals the space. Afterward, your dentist will place a crown on the tooth to protect and restore it to its original function.What is filled in root canal?
The root canal is filled with a rubberlike substance called gutta-percha. This acts as a permanent bandage. It prevents bacteria or fluid from entering the tooth through the roots. Typically, the opening in the tooth is then closed with a temporary crown or filling.
What is Pulpal diagnosis?Pulpal Normal pulp A clinical diagnostic category in which the pulp is symptom-free and normally responsive to pulp testing. Reversible pulpitis A clinical diagnosis based on subjective and objective findings indicating that the inflammation should resolve and the pulp return to normal.
Article first time published onWhat is pulp vitality test?
Pulp vitality tests attempt to examine the presence of pulp blood flow, as this is viewed as a better measure of true health than sensibility. Laser Doppler flowmetry and pulse oximetry are examples of vitality tests.
What is percussion pain?
Percussion pain or tenderness is generally interpreted as a sign of apical inflammation. Since this is usually caused by bacterial infection of necrotic pulp tissue, percussion tenderness may indirectly indicate a non-vital pulp.
What is acute pulpitis?
Pulpitis is a condition that causes painful inflammation of the pulp. It can occur in one or more teeth, and is caused by bacteria that invade the tooth’s pulp, causing it to swell. There are two forms of pulpitis: reversible and irreversible.
How are endodontics diagnosed?
In order to render proper treatment, a complete endodontic diagnosis must include both a pulpal and a periapical diagnosis for each tooth evaluated. Endodontic diagnosis is similar to a jigsaw puzzle—diagnosis cannot be made from a single isolated piece of information (4).
What is coronal pulp?
The portion of the dental pulp in the pulp chamber or in the crown of the tooth.
How do you treat Perio Endo lesions?
The treatment for primary endo lesions involves nonsurgical root canal therapy and appropriate restorative care. In these cases, periodontal intervention is not necessary, and outcomes for these teeth are quite predictable.
What is the best mouthwash to use for periodontal disease?
- Best Overall: TheraBreath Healthy Gums Periodontist Formulated 24-Hour Oral Rinse. …
- Best Budget: ACT Anticavity Zero Alcohol Fluoride Mouthwash. …
- Best Alcohol-Free: Listerine Zero Cool Mint Mouthwash. …
- Best Sensitive: CloSYS Ultra Sensitive Mouthwash. …
- Best for Dry Mouths: Colgate Hydris Dry Mouth Mouthwash.
What is a PARL in dental?
Periapical radiolucency is the descriptive term for radiographic changes which are most often due to apical periodontitis and radicular cysts, that is, inflammatory bone lesions around the apex of the tooth which develop if bacteria are spread from the oral cavity through a caries-affected tooth with necrotic dental …
Is root canal painful?
During root canal therapy, the pulp is removed, and the inside of the tooth is cleaned and sealed. People fear root canals because they assume they are painful. Actually, most people report that the procedure itself is no more painful than having a filling placed.
Why are root canals bad for you?
Accumulation of unwanted materials: Cholesterol crystals can accumulate and irritate the tissues where the root canal was done, as well as scar tissue or cystic lesions. Immune system response: The procedure can cause an overactive immune response in your body, causing negative health impacts.
Can a root canal fell out?
What to Do When a Root Canal Filling Falls Out. Root canal filling seals saliva out of your tooth and prevents reinfection and root canal failure. If you leave the tooth untreated, fluid and saliva will leak into it and loosen the root canal filler material. When root canal filling falls out, a dentist must replace it.
Does gutta percha hurt?
The result is a lot of postoperative pain once the anesthesia wears off. Then, to make matters worse, the gutta-percha is now pushed through the anatomic apex and sealed into the ligament and bone. No wonder it sometimes does not heal and often causes the patient discomfort.
Does a root canal remove the nerve?
Do you kill my nerves during endodontic (root canal) treatment? No, the nerves are not “killed” during endodontic treatment. Inflamed or infected pulp tissue, containing nerves and blood vessels, is removed from the pulp chamber of a tooth.
Are crowns painful?
Getting a crown shouldn’t cause you any more pain or discomfort than a typical filling. Your dentist will make sure that they put a local numbing jelly on your teeth, gums and surrounding tissues, but there is usually an anesthetic injected as well, so you might feel a small pinch.
What are the 3 stages of root canal treatment?
- Extirpation: Initial clean to control bacterial infection. …
- Instrumentation: Thorough clean and medicine. …
- Obturation: Filling the root canal.
Is a crown necessary after a root canal?
After a root canal, they can simply be restored with dental filling and left without a crown. However, if the front tooth has been discolored by decay, then a crown should be fitted for cosmetic purposes.
How do I know if my pulp is infected?
- Intense pain.
- Spontaneous pain.
- Sensitivity to cold that lasts more than 30 seconds.
- Sensitivity to heat.
- Pain when the tooth is tapped.
- Swelling around tooth and gums.
- Fever.
- Bad breath.
What is the treatment for Pulpitis?
Treatment involves removing decay, restoring the damaged tooth, and sometimes doing root canal therapy or extracting the tooth. Reversible: Pulpitis begins as limited inflammation, and the tooth can be saved by a simple filling.
Can Pulpitis be seen on xray?
No changes around the end of the root will be seen on the X-ray in early pulpitis; the tooth radiographically will appear normal. However, teeth that have become infected and have lost their vitality (i.e. the nerve has died) can show a range of changes.
What is the temperature of Endo ice?
PERFECT FOR TESTING PULP VITALITY! Cold as Ice Endo Spray is perfect for on the spot testing of pulp health. The endo spray causes a rapid pulpal response in vital teeth due to its low liquid temperature of -26.2°C (-15.2°F).
Is a pulp test painful?
a)Normal Response: Healthy pulps are expected to respond to sensitivity testing by eliciting a short, sharp pain which subsides when the stimulus is removed, indicating that the nerve fibres are present and responsive.