What is expiratory trigger sensitivity

Sarah Rodriguez
Published Feb 25, 2026
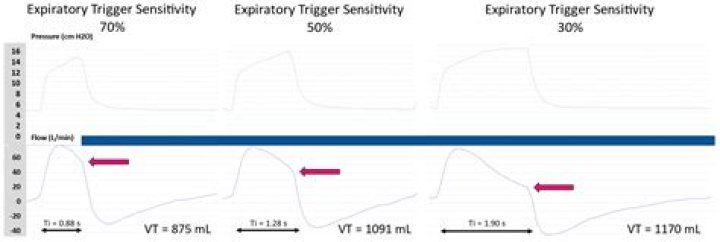
The expiratory trigger sensitivity (ETS) is the percentage of peak inspiratory flow that controls the expiratory valve open- ing and the cycling to expiration. It can be manually set from minimum values of 5% to a maximum of 60%–70% of the peak flow; the default setting is usually at 25% of the peak flow.
What is expiratory sensitivity?
Expiratory sensitivity (ESENS) sets the percentage of delivered peak inspiratory flow necessary to terminate inspiration and initiate exhalation. The clinician determines the ESENS setting, adjustable from 1% to 80%. A lower ESENS setting increases inspiratory time. A higher ESENS setting decreases inspiratory time.
What is sensitivity setting on ventilator?
On Hamilton Medical ventilators, the setting for the expiratory trigger is the expiratory trigger sensitivity (ETS). This value represents the percent of peak inspiratory flow at which the ventilator cycles from inspiration to exhalation. On Hamilton Medical ventilators, ETS can be set to anywhere between 5% and 80%.
What is trigger sensitivity?
The sensitivity of the trigger determines how much effort the patient has to exert before his inspiration is augmented by the ventilator.What is trigger in ventilator?
Triggering refers to the signal that causes inspiration. A ventilator breath may be time triggered or patient triggered. During patient-triggered breaths, the ventilator may detect patient effort using a variety of inputs. These include pressure, volume, flow, impedance, and motion.
What is trigger BiPAP?
The trigger phase variable determines how a mechanical breath is initiated. This variable determines whether a mode of ventilation can be described as “mandatory” or “spontaneous”.
What is expiratory sensitivity in ventilator?
The expiratory trigger sensitivity (ETS) is the percentage of peak inspiratory flow that controls the expiratory valve open- ing and the cycling to expiration. It can be manually set from minimum values of 5% to a maximum of 60%–70% of the peak flow; the default setting is usually at 25% of the peak flow.
What trigger means?
1a : to release or activate by means of a trigger especially : to fire by pulling a mechanical trigger trigger a rifle. b : to cause the explosion of trigger a missile with a proximity fuse. 2 : to initiate, actuate, or set off by a trigger an indiscreet remark that triggered a fight a stimulus that triggered a reflex.What triggers trigger trigger and pressure?
In a pressure-triggered mode, the ventilatory support detects the drop in airway pressure that occurs with inspiratory effort. Flow triggering was designed to avoid the decrease in airway pressure that occurs with pressure triggering and, therefore, increases the work of breathing.
What can happen if I set the trigger too sensitive?As described above, a too sensitive ventilator causes excessive triggering that can interfere with ventilation and can increase the risk of hyperinflation, barotrauma, hemodynamic instability and hyperventilation during assist-control or high levels of pressure support ventilation.
Article first time published onWhat is P ramp ventilator?
The ‘ramp’ option is a comfort setting initially made available on CPAP devices. This option exists in pressure-cycled ventilators, allowing a progressive increase of expiratory positive airway pressure (EPAP) only.
What are the settings on a ventilator?
Almost all ventilators have the capability of being set to four basic modes: AC, synchronized intermittent mandatory ventilation (SIMV), airway pressure release ventilation (APRV), and pressure support (PS).
What is pressure limit?
In pressure-controlled ventilation, a pressure limit is the control variable for the respiratory cycle. … This does not end the inspiratory phase; rather, the pressure is maintained at this limit by a decreasing flow.
How does flow trigger work?
When the patient makes an inspiratory effort, some of the gas that was previously flowing continuously through the circuit is diverted to the patient. The ventilator senses the decrease in flow returning through the circuit, and a breath is triggered.
How many triggering types are available in mechanical ventilator?
Currently, patient-triggered ventilation can occur by 4 methods: pressure triggering, flow triggering, volume triggering, or shape-signal triggering.
What is expiratory pause?
The expiratory hold pauses the breath in expiration, preventing the delivery of more breaths. With the flow stopped, alveolar pressure equilibrates with the ventilator circuit and can be measured.
Who uses BiPAP?
Bilevel positive airway pressure (BiPAP) is a type of noninvasive ventilation. It is used when you have a condition that makes it hard to breathe like sleep apnea, COPD, asthma, heart conditions and other ailments.
What is IE ratio ventilation?
The I:E ratio denotes the proportions of each breath cycle devoted to the inspiratory and expiratory phases. The duration of each phase will depend on this ratio in conjunction with the overall respiratory rate. … Increasing the I:E ratio to 1:3 will result in 1.5 seconds of inspiration and 4.5 seconds of expiration.
How can I improve my synchrony?
Patient-ventilator synchrony can be improved with proper adjustment of ventilator settings, cautious administration of sedatives, and use of modes with that provide continuous spontaneous ventilation with servo targeting (ie, inspiratory pressure proportional to inspiratory effort26,27).
What is the difference between NIV and ventilator?
In invasive ventilation, air is delivered via a tube that is inserted into the windpipe through the mouth or sometimes the nose. In NIV, air is delivered through a sealed mask that can be placed over the mouth, nose or the whole face.
What is CPAP mode?
Continuous positive airway pressure (CPAP) is one of two cardinal modes of noninvasive ventilation. It provides one continuous pressure throughout the respiratory cycle—the pressure is set to the same level for inspiration and expiration.
Why is BiPAP better than CPAP?
Exhaling can be challenging for some patients who are using CPAP devices at higher pressures. But using a BiPAP machine, patients can breathe easier as the machine reduces the pressure level during exhalation, allowing the patient to exhale more easily and breathe more comfortably.
What does Simv stand for?
Introduction. Synchronized intermittent mandatory ventilation (SIMV) is a type of volume control mode of ventilation. With this mode, the ventilator will deliver a mandatory (set) number of breaths with a set volume while at the same time allowing spontaneous breaths.
What flowrate is required to trigger on a breath?
High peak flow rates increase peak airway pressures and lower mean airway pressures, which may decrease oxygenation. In most patients, peak flow rates of 60 L/min are adequate.
What is the example of trigger?
Trigger is defined as to fire a gun or to start a series of events or emotions. An example of trigger is to shoot a rifle while hunting. An example of trigger is to start crying at a movie, thereby causing many other people in the theater to begin weeping.
What does getting triggered mean?
To be triggered is to have an intense emotional or physical reaction, such as a panic attack, after encountering a trigger. Related words: content warning.
What happens when someone is triggered?
A trigger is a reminder of a past trauma. This reminder can cause a person to feel overwhelming sadness, anxiety, or panic. It may also cause someone to have flashbacks. A flashback is a vivid, often negative memory that may appear without warning.
What is Simv mode of ventilation?
Synchronized intermittent mandatory ventilation (SIMV) is a type of volume control mode of ventilation. With this mode, the ventilator will deliver a mandatory (set) number of breaths with a set volume while at the same time allowing spontaneous breaths.
What is the difference between Pip and plateau pressure?
Paw is airway pressure, PIP is peak airway pressure, Pplat is plateau pressure. Some researchers have suggested that plateau pressures should be monitored as a means to prevent barotrauma in the patient with ARDS. Plateau pressures are measured at the end of the inspiratory phase of a ventilator-cycled tidal volume.
What is PIP in ventilator?
From Wikipedia, the free encyclopedia. Peak inspiratory pressure (PIP) is the highest level of pressure applied to the lungs during inhalation. In mechanical ventilation the number reflects a positive pressure in centimeters of water pressure (cmH2O).
What is PIP and PEEP?
The difference between PEEP set and the pressure measured during this maneuver is the amount of auto-PEEP. PIP = peak inspiratory pressure. As illustrated here, the measured auto-PEEP can be considerably less than the auto-PEEP in some lung regions if airways collapse during exhalation.