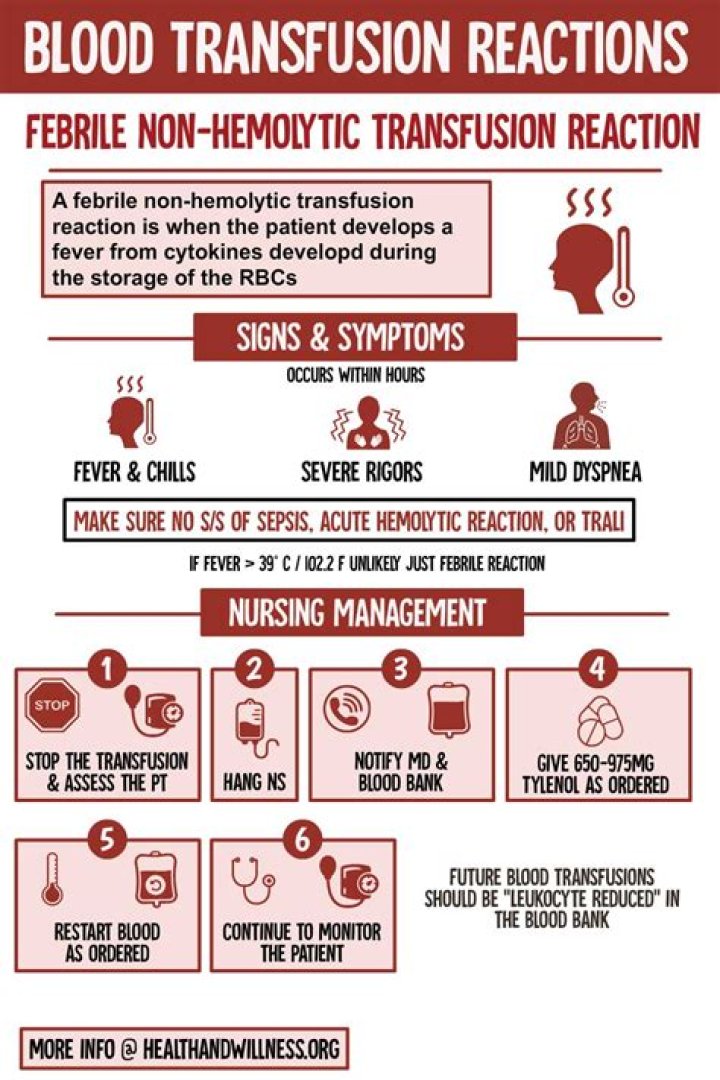
What is febrile Nonhemolytic transfusion reaction

Dylan Hughes
Published Apr 18, 2026
Febrile nonhemolytic transfusion reactions (FNHTRs) are common, occurring with 1–3% of transfusions. FNHTR manifests as fever and/or chills without hemolysis occurring in the patient during or within 4 hours of transfusion cessation. Diagnosis is made by excluding other causes of fever.
What is a febrile reaction to blood transfusion?
Febrile reactions Cause: Fever and chills during transfusion are thought to be caused by recipient antibodies reacting with white cell antigens or white cell fragments in the blood product or due to cytokines which accumulate in the blood product during storage.
What is the meaning of febrile reaction?
Definition of febrile : marked or caused by fever : feverish a febrile reaction caused by an allergy.
What causes a febrile transfusion reaction?
Nonhemolytic febrile transfusion reactions are usually caused by cytokines from leukocytes in transfused red cell or platelet components, causing fever, chills, or rigors. In the transfusion setting, a fever is defined as a temperature elevation of 1º C or 2º F.How does one prevent febrile Nonhemolytic transfusion reactions?
Possible interventions include prestorage leukoreduction, plasma removal from the platelet product before transfusion, and reduction of the platelet storage period to 3 days. Clinical studies to identify the most effective approach for preventing febrile nonhemolytic transfusion reactions have not yet been reported.
How do you prevent a febrile transfusion reaction?
The best way to prevent severe febrile reactions is to use prestorage leukocyte reduced red blood cells and apheresis platelets. If a patient continues to have febrile reactions to leukocyte reduced single donor platelets, it may be helpful to remove plasma from the platelet unit immediately prior to transfusion.
How is a febrile transfusion reaction treated?
In febrile, nonhemolytic reactions, fever usually resolves in 15-30 minutes without specific treatment. If fever causes discomfort, oral acetaminophen (325-500 mg) may be administered. Avoid aspirin because of its prolonged adverse effect on platelet function.
What should the nurse do if a transfusion reaction is suspected?
- Stop the transfusion.
- Keep the I.V. line open with normal saline solution.
- Notify the physician and blood bank.
- Intervene for signs and symptoms as appropriate.
- Monitor the patients vital signs.
What happens during a transfusion reaction?
A hemolytic transfusion reaction is a serious complication that can occur after a blood transfusion. The reaction occurs when the red blood cells that were given during the transfusion are destroyed by the person’s immune system. When red blood cells are destroyed, the process is called hemolysis.
What does Nonhemolytic mean?Definition of nonhemolytic medical. : not causing or characterized by hemolysis : not hemolytic a nonhemolytic streptococcus.
Article first time published onWhich of the following are symptoms of FNHTR?
Chills, rigors, increased respiratory rate, change in blood pressure, anxiety and a headache may accompany this reaction but occur in several more serious transfusion reactions also, the most serious being acute haemolytic reaction, transfusion associated sepsis and TRALI.
What is the meaning of Alloimmunization?
Alloimmunization is defined as an immune response to foreign antigens after exposure to genetically different cells or tissues. Although alloimmunization is a natural event during pregnancy, frequently it is the undesirable outcome of a blood transfusionand/or transplant.
What is the most common transfusion reaction?
Febrile non-hemolytic transfusion reactions are the most common reaction reported after a transfusion. FNHTR is characterized by fever or chills in the absence of hemolysis (breakdown of red blood cells) occurring in the patient during or up to 4 hours after a transfusion.
How do you evaluate a transfusion reaction?
The initial hemolytic transfusion reaction evaluation consists of a clerical check to verify proper patient and unit identification, a visual check of patient plasma for hemolysis, and a direct antiglobulin test.
Can you transfuse a febrile patient?
With physician approval, a transfusion may be administered to a febrile patient. However, if a patient is febrile, consideration should be given to postponement of the blood transfusion, since the fever may mask the development of a febrile reaction to the blood component itself.
How do you manage a transfusion reaction?
- Stop the transfusion immediately and activate emergency procedures if required.
- Check and monitor the patient’s vital signs.
- Maintain intravenous (IV) access (do not flush the existing line and use a new IV line if required).
How long does it take for platelets to increase after transfusion?
Significant increases in posttransfusion platelet increments were associated with prior splenectomy at both 1 and 18 to 24 hours after transfusion. Older patient age was also associated with increased platelet increments but only at 1 hour after transfusion.
Why normal saline is used in blood transfusion?
Background: It is standard practice at many hospitals to follow blood component transfusions with a normal saline (0.9% NaCl) flush. This serves the dual purpose of administering to the patient any residual blood left in the administration set (up to 40 mL), and it flushes the line for later use.
What is the first step to a blood transfusion reaction?
Transfusion reactions require immediate recognition, laboratory investigation, and clinical management. If a transfusion reaction is suspected during blood administration, the safest practice is to stop the transfusion and keep the intravenous line open with 0.9% sodium chloride (normal saline).
Why is furosemide given after blood transfusion?
For many years, furosemide has been used routinely by physicians during and after blood transfusions in neonates and other age groups. The rationale behind this common practice is to reduce the vascular overload that may be imposed by the additional blood volume delivered during transfusion.
How is circulatory overload treated?
Patients should be treated with supplemental oxygen. An attempt may be made to reduce the intravascular plasma volume with diuretics. Placing the patient in a sitting position may be additionally helpful. If symptoms do not abate with the aforementioned steps, diuretics may be repeated.
Which of the following diseases occur after a streptococcal infection?
PSGN is a kidney disease that can develop after infections caused by bacteria called group A Streptococcus (group A strep). These infections include throat and skin infections like strep throat, scarlet fever, and impetigo.
Who is at risk for febrile non hemolytic transfusion reaction?
FNHTRs are more common in the transfusion of platelets. Multiply-transfused patients and multiparous women make up the largest populations experiencing this type of reaction. There are two mechanisms involved in the manifestation of an FNHTR.
What is the incidence of Nonhemolytic transfusion reaction?
FNHTRs are the most common compli- cation of platelet transfusion. 1. Incidence ranges from 1.7% to 31%.
What is alloimmunization in blood transfusion?
Alloimmunization consists of the induction of immunity in response to foreign antigen(s) encountered through exposure to cells or tissues from a genetically different member of the same species.[1] It is one of the major complications of regular blood transfusions, particularly in patients who are chronically …
How is alloimmunization diagnosed?
Alloimmunization may be diagnosed based upon signs and symptoms of a reaction, ultrasounds during pregnancy, or blood sample antibody testing.
How do you treat alloimmunization?
Plasmapheresis (eg, 2 plasma volumes for 1-3 d) before bone marrow transplantation results in beneficial responses in most patients who are alloimmunized to platelets. Perfusion of the plasma through a staphylococcal protein A column is an experimental treatment that has met with some success.
Why do you need a urine sample after a transfusion reaction?
In allergic reactions, the presence of red plasma or urine, discordant pretransfusion and posttransfusion ABO blood types, or a positive antiglobulin (Coombs) test indicates other diagnoses in addition to an allergic reaction.
What is bacterial transfusion reaction?
Clinical features suggesting the possibility of bacterial contamination and/or endotoxin reaction may include rigors, high fever, severe chills, hypotension, tachycardia, nausea and vomiting, dyspnoea, or circulatory collapse during or soon after transfusion.
Can platelets cause transfusion reaction?
The reported incidence of adverse reactions to platelet transfusion ranges from 5% to 31% (8,11). In a recent prospective study, Heddle et al. reported adverse reactions in 30.8% of platelet transfusions versus 6.8% of red cell transfusions (11).



