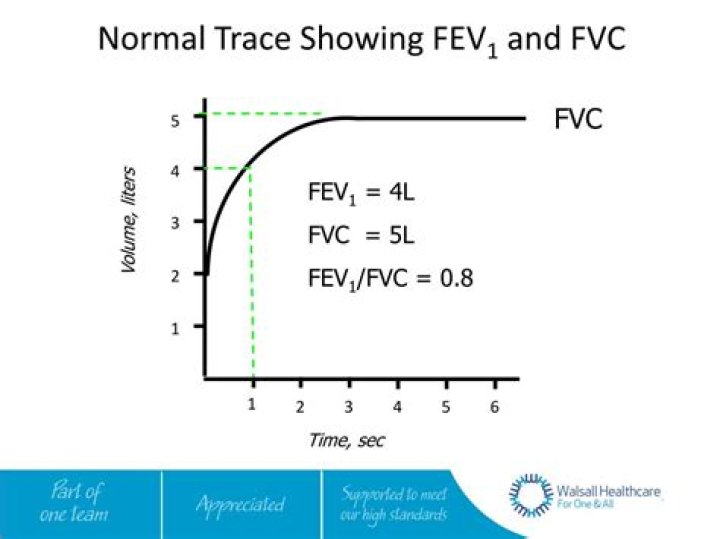
What is normal FVC

Nathan Sanders
Published Mar 01, 2026
Pulmonary function testNormal value (95 percent confidence interval)FVC80% to 120%Absolute FEV1 /FVC ratioWithin 5% of the predicted ratioTLC80% to 120%FRC75% to 120%
What is an abnormal FVC?
Restrictive lung diseases can cause the FVC to be abnormal. This means that the lung is restricted from filling to its normal capacity of air. Asbestosis (scarring of the lung due to asbestos exposure) is an example of a restrictive lung disease.
What is FVC for lungs?
Forced vital capacity (FVC) is the total amount of air exhaled during the FEV test. Forced expiratory volume and forced vital capacity are lung function tests that are measured during spirometry. Forced expiratory volume is the most important measurement of lung function.
What is a low FVC?
Diminished FVC Forced vital capacity can be decreased temporarily or permanently. A diminished FVC value is a sign of several conditions, including: Chronic obstructive pulmonary disease (COPD), including chronic bronchitis, emphysema, and bronchiectasis.Is FVC normal in COPD?
In patients with COPD, post-bronchodilator FEV1/FVC remains < 0.7. However, the FEV1 may improve significantly after bronchodilator, and a change of > 12% AND > 200 mL in FEV1 can occur in COPD1.
What is a normal reading on a spirometer?
Percentage of predicted FEV1 valueResult80% or greaternormal70%–79%mildly abnormal60%–69%moderately abnormal50%–59%moderate to severely abnormal
What is a good score on a spirometry test?
Normal results are 70% or more for adults under 65. FVC/FEV-1 ratios below normal help your doctor rate the severity of your lung condition: Mild lung condition: 60% to 69% Moderate lung condition: 50% to 59%
What is a good lung function test result?
Lung volume is measured in litres. Your predicted total lung capacity (TLC) is based on your age, height, sex and ethnicity, so results will differ from person to person. Normal results typically range between 80% and 120% of the prediction.How can I improve my FVC?
Many studies have shown that FVC is significantly improved after high-intensity aerobic exercise. This means that the vital capacity also increased.
What FVC expired in 1 second means?The forced expiratory volume in 1 second (FEV1) is the volume of air (in liters) exhaled in the first second during forced exhalation after maximal inspiration. Normally, at least 80% of the forced vital capacity (FVC) is exhaled in the first second.
Article first time published onWhat does 80 percent lung capacity mean?
Forced vital capacity: the maximum amount of air you can forcibly exhale from your lungs after fully inhaling. It is about 80 percent of total capacity, or 4.8 liters, because some air remains in your lungs after you exhale.
Is FVC reduced in asthma?
In summary, reversibility of airflow obstruction in asthma is defined by an increase in FEV1 of 12% or 200 ml. There is generally an increase in FEV1/FVC since FVC changes less than FEV1, making FVC a less useful parameter for assessing reversibility.
How can I test my lung capacity at home?
How do you measure your lung capacity? A common method is using a Peak Flow Meter, a handheld device that measures the strength of your breath. You simply breathe into one end and the meter instantly shows a reading on a scale, typically in liters per minute (lpm).
What percentage should your lung capacity be?
Your predicted total lung capacity (TLC) is based on your age, height, sex and ethnicity, so results will differ from person to person. Normal results typically range between 80% and 120% of the prediction.
What is lung Exerciser?
The breaths you take may not be as deep as usual. That means the air in your lungs may not move much and may not clear out any infections. You inhale through an incentive spirometer to exercise your lungs and to get air into every nook and cranny. Your doctor may also call it a manual incentive spirometer.
What is considered a low DLCO?
Normal and Critical Findings Normal DLCO: >75% of predicted, up to 140% Mild: 60% to LLN (lower limit of normal) Moderate: 40% to 60% Severe: <40%
Does walking increase lung capacity?
Both aerobic activities and muscle-strengthening activities can benefit your lungs. Aerobic activities like walking, running or jumping rope give your heart and lungs the kind of workout they need to function efficiently.
Can lung capacity be increased?
“A certain amount of increased lung capacity can be gained from physical exercise that involves heavy or deep breathing,” said Dr. Martin. “However, the benefits of exercise come mostly from improvements in muscle function, blood flow, and cardiac function.”
Does exercise affect FVC?
In general regular exercise does not substantially change measures of pulmonary function such as total lung capacity, the volume of air in the lungs after taking the largest breath possible (TLC), and forced vital capacity, the amount of air able to be blown out after taking the largest breath possible (FVC).
Is a peak flow of 250 good?
Normal adult peak flow scores range between around 400 and 700 litres per minute, although scores in older women can be lower and still be normal. The most important thing is whether your score is normal for you.
Why is my lung capacity so low?
Age, smoking, pollution, and other factors can cause the lungs to work less efficiently. Certain health problems can restrict the lungs’ capacity, such as chronic obstructive pulmonary disease (COPD) and asthma. A person may not be able to change how much oxygen their lungs can hold.
How can you tell if you have a lung infection?
- imaging, such as a chest X-ray or CT scan.
- spirometry, a tool that measures how much and how quickly you take in air with each breath.
- pulse oximetry to measure the level of oxygen in your blood.
- taking a sample of mucus or nasal discharge for further testing.
Which is more important FVC or FEV1?
FVC was not associated with overall mortality. For most COPD criteria sensitivity was low and specificity high. The area under the curve for FEV1 was greater than for FVC for overall and cardiovascular mortality.
How do you calculate FVC?
- FEV1 = Race x 1.08 x [(0.0395 x Height) – (0.025 x Age) – 2.6]
- FVC = Race x 1.15 x [(0.0443 x Height) – (0.026 x Age) – 2.89]
- FEV1/FVC Ratio = FEV1 / FEVC.
What is your total lung capacity?
Lung capacity or total lung capacity (TLC) is the volume of air in the lungs upon the maximum effort of inspiration. Among healthy adults, the average lung capacity is about 6 liters. Age, gender, body composition, and ethnicity are factors affecting the different ranges of lung capacity among individuals.
How bad is 30 Lung function?
30% to 49%. At this level, the lungs are not working well at all. Less than 30%. People at this stage get out of breath with just a little activity.
How long can you live with 40 percent lung capacity?
The 5-year life expectancy for people with COPD ranges from 40% to 70%, depending on disease severity. This means that 5 years after diagnosis 40 to 70 out of 100 people will be alive. For severe COPD, the 2-year survival rate is just 50%.
Are large lungs good or bad?
Lungs can be too large, they caution. If lungs are beyond a certain size, surgeons could have trouble closing the chest cavity, the lungs could be too compressed and collapse or could weigh too heavily on the heart, causing low blood pressure and other problems.
What are the symptoms of weak lungs?
- Trouble breathing.
- Shortness of breath.
- Feeling like you’re not getting enough air.
- Decreased ability to exercise.
- A cough that won’t go away.
- Coughing up blood or mucus.
- Pain or discomfort when breathing in or out.
What do damaged lungs feel like?
Coughing up blood: If you are coughing up blood, it may be coming from your lungs or upper respiratory tract. Wherever it’s coming from, it signals a health problem. Chronic chest pain: Unexplained chest pain that lasts for a month or more—especially if it gets worse when you breathe in or cough—also is a warning sign.
How can I test myself for COPD?
It’s simple and painless. You will be asked to take a deep breath, and you’ll blow hard into a mouthpiece that’s connected to a small machine. That machine, called the spirometer, measures how fast you blow air out of your lungs. Results can tell you whether you have COPD, even if you haven’t gotten symptoms yet.



