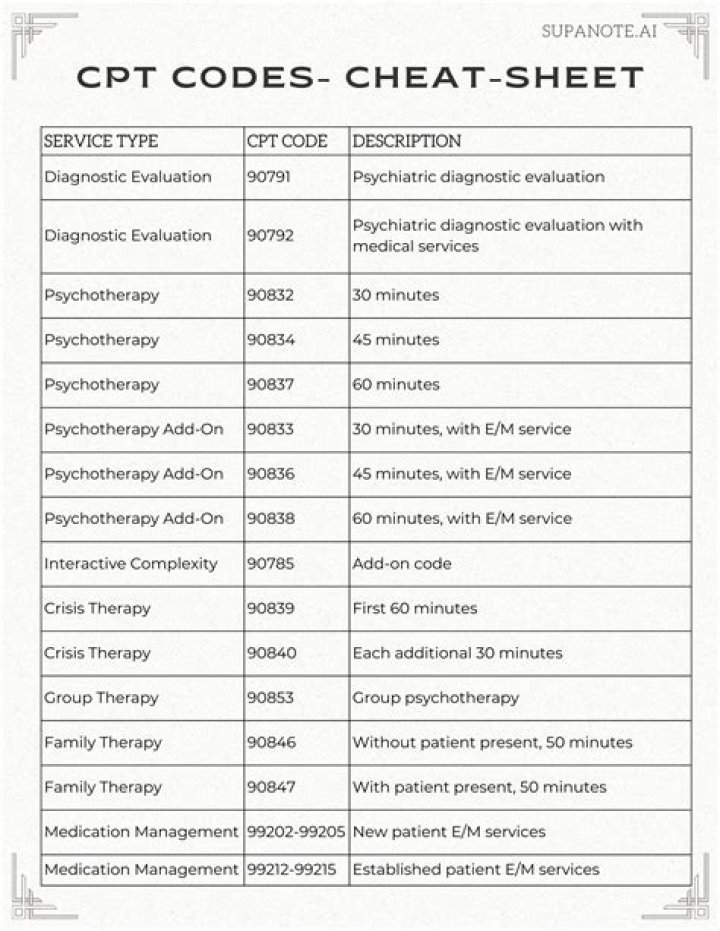
What is the CPT code for telephone calls

Rachel Hunter
Published Apr 12, 2026
CPT CodeTimeModifiersG20125-10 minN/A994415-10 minN/A9944211-20 minN/A9944321-30 minN/A
Can you bill for patient phone calls?
The phone call must be for analysis or decision making that requires the physician. In other words, you should not be billing for a patient phone call that is simply to request to reschedule an upcoming office visit.
What is the difference between 99421 and 99441?
True Blue. If you are referring to 99421-99423, those are for ONLINE services only. If you are performing telephone encounters, 99441-99443 are the codes you are looking for. Please note these are for established patients only.
Can an RN bill for telephone calls?
Answer: An RN can provide Telephone Triage calls when the RN is overseen by a physician, NP or PA. The Telephone Triage calls can be billed using CPT codes 98966-98968; the rendering requirement provider information on the claim must reflect the overseeing provider’s NPI and/or Medicaid Provider ID number.Can 99358 be used for telephone calls?
Non-Face-to-face prolonged service codes, 99358‒99359 can be billed with telephone services (99443 and 98968 would be reported for the first 30 minutes). 99358‒99359 are also allowed for telehealth visits.
What is the CPT code 99211?
Code 99211 is commonly used for services such as patient education, simple rechecks and medication reviews. … A patient comes to the office for a blood-pressure check. If the visit was scheduled at the request of the physician, 99211 should be reported.
What is procedure code 99441?
99441: telephone E/M service; 5-10 minutes of medical discussion. 99442: telephone E/M service; 11-20 minutes of medical discussion.
Does Medicare pay for 99441?
Medicare payment for the telephone evaluation and management visits (CPT codes 99441-99443) is equivalent to the Medicare payment for office/outpatient visits with established* patients effective March 1, 2020.What modifier is used for a telephone visit?
Physicians should append modifier -95 to the claim lines delivered via telehealth. Claims with POS 02 – Telehealth will be paid at the normal facility rate, which is typically less than the non-facility rate under the Medicare physician fee schedule.
Are telephone encounters billable?Telephone services (99441-99443) These codes can only be reported for an established patient and are not billable if the call results in the patient coming in for a face-to-face service within the next 24 hours (or next available urgent visit).
Article first time published onWhat is the CPT code for telehealth?
Telephone visits and audio-only telehealth Telehealth CPT codes 99441 (5-10 minutes), 99442 (11-20 minutes), and 99443 (20-30 minutes)
What is the reimbursement for 99441?
CodeNon-Facility FeeFacility Fee99441$46.13$26.3199442$76.04$52.2699443$110.28$80.37
What CPT codes do you use for telemedicine?
We’ve found that most payers advise providers billing telemedicine to use the appropriate evaluative and management CPT code (99201 – 05, 99211-15) along with a GT or 95 modifier (more on that below).
What does CPT code 99080 mean?
The CPT code 99080 is for special reports such as insurance forms, more than the information conveyed in the usual medical communications or standard reporting form. As stated in the code descriptor, this code is used for things such as insurance forms (for life insurance or new health insurance).
What is procedure code 99215?
The CPT evaluation and management (E/M) code 99215, “Office or other outpatient visit for an established patient,” is rarely used, accounting for about 5 percent of E/M visits.
Can CPT code 99358 be billed alone?
Beginning calendar year (CY) 2017, these codes are separately payable under the Medicare Physician Fee Schedule. Additionally, these codes (99358-99359): Cannot be reported during the same service period as complex chronic care management (CCM) services or transitional care management services.
Do phone calls count as telehealth?
Reminder: phone calls are not telehealth, so do not add the modifier -95.
What does CPT code 99443 mean?
CPT 99441 – 5-10 minute medical discussion. CPT 99442 – 11-20 minute medical discussion. CPT 99443 – 21-30 minute medical discussion. CPT 99091 – Collection and interpretation of physiologic data, digitally stored and/ or transmitted by the patient to the physician, requiring a minimum of 30 minutes of time.
What is modifier GT?
The GT modifier is used to indicate the session was administered via a telecommunications system. The reason the GT modifier is used is to signify to the insurance company the delivery of your services has changed (i.e. over video call).
Does Medicare pay for 99211?
Does Medicare Approve 99211? Yes, Medicare considers this routine. If you are an approved Medicare provider you can bill this code.
Is 99211 a valid CPT code for 2021?
CPT code 99211 (established patient, level 1) will remain as a reportable service.
What is level 4 office visit?
CPT defines a 99214 or level-IV established patient visit as one involving a detailed history, detailed examination and medical decision making of moderate complexity. … This means that the coding can be based on the extent of the history and medical decision making only.
What is the difference between modifier 95 and modifier GT?
95 Modifier Modifier 95 is similar to GT in use cases, but, unlike GT, there are limits to the codes that it can be appended to. Modifier 95 was introduced in January 2017, and it is one of the newest additions to the telemedicine billing landscape.
What is the difference between modifier GT and 95 2020?
95 Modifier vs. A GT modifier is an older coding modifier that serves a similar purpose as the 95 modifier. CMS recommends 95, different companies have varying standards for which codes to be billed. It is a good idea to check with the plans before billing.
What is the difference between CPT code G2012 and 99441?
Q: We cannot seem to settle this debate at my obstetrics/gynecology office: What is the difference between G2012 and 99441? A: The codes are very similar. One is an HCPCS code and the other is the first of three CPT diagnostic codes.
Does Medicare pay for phone call visits?
You can get Medicare telehealth services for certain emergency department visits at home. You can get certain physical and occupational therapy services at home. Medicare covers some services delivered via audio only devices. Medicare also covers virtual check-ins and E-visits.
What is CPT code 99444?
99444 Online evaluation and management service provided by a physician or other qualified health care professional who may report evaluation and management services provided to an established patient or guardian, not originating from a related E/M service provided within the previous 7 days, using the internet or …
Does Medicare accept consultation codes?
Medicare does not accept claims for either outpatient (99241-99245) or inpatient (99251-99255) consultations, and instead requires that services be billed with the most appropriate (non-consultation) E/M code.
What is difference between telehealth and telemedicine?
Telehealth refers broadly to electronic and telecommunications technologies and services used to provide care and services at-a-distance. What’s the difference? … Telemedicine refers specifically to remote clinical services, while telehealth can refer to remote non-clinical services.
Which code Cannot be reported as a telemedicine code?
Scenario 1: Telehealth Visit practitioner cannot use CPT codes 99202-99205. These codes are used only when audio and video are used for the visit. Instead, use CPT codes 99441-99443 with Modifier CR.
What does CPT code 99070 mean?
Unlisted Supplies and Materials (CPT® Code 99070) CPT procedure 99070 is the code to bill for physicians’ unlisted supplies and materials used in non-surgical procedures. If more than one claim line for 99070 is used for the same date of service, the additional line(s) will be denied.