What is the mechanism of action of anticoagulant medications quizlet

Lily Fisher
Published Apr 23, 2026
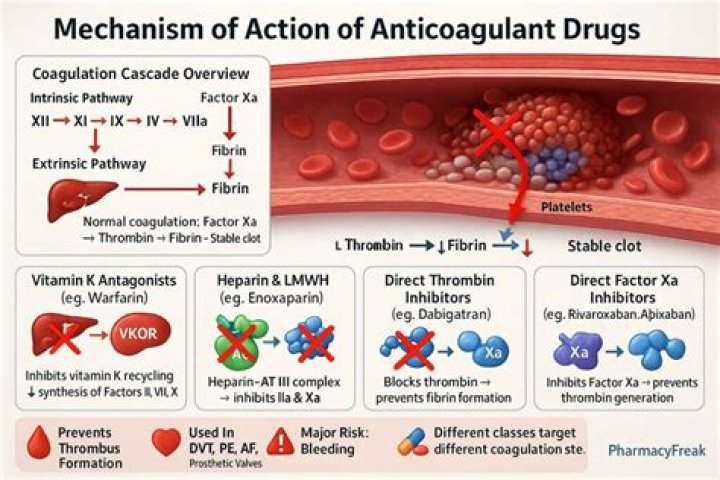
Anticoagulants achieve their effect by suppressing the synthesis or function of various clotting factors that are normally present in the blood. Such drugs are often used to prevent the formation of blood clots (thrombi) in the veins or arteries or the enlargement of a clot that is circulating in the bloodstream.
What is the mechanism of action for anticoagulants?
Anticoagulants achieve their effect by suppressing the synthesis or function of various clotting factors that are normally present in the blood. Such drugs are often used to prevent the formation of blood clots (thrombi) in the veins or arteries or the enlargement of a clot that is circulating in the bloodstream.
What are examples of anticoagulants?
- apixaban (Eliquis)
- dabigatran (Pradaxa)
- edoxaban (Lixiana)
- rivaroxaban (Xarelto)
- warfarin (Coumadin)
What is the function of an anticoagulant?
Anticoagulants are medications that help stop your blood from thickening or “clotting.” Your body does need to be able to clot to help seal wounds inside and outside your body. But unnecessary clots can cause problems that can be life-threatening.What is anticoagulant in pharmacology?
Anticoagulants are used to prevent the formation or growth of fibrin/erythrocyte thrombi in the venous circulation. They are not useful for treating arterial thrombi which are mainly composed of platelet aggregates. Anticoagulants can be administered parenterally or orally.
What is the mechanism of action of heparin?
Mechanism of action Heparin binds to the enzyme inhibitor antithrombin III (AT), causing a conformational change that results in its activation through an increase in the flexibility of its reactive site loop. The activated AT then inactivates thrombin, factor Xa and other proteases.
What is the mechanism of action of the anticoagulants heparin and warfarin?
These proteins are called “cofactors.” Vitamin K controls the creation of these cofactors in your liver, and warfarin reduces clotting in your blood by preventing vitamin K from working correctly. Heparin also works by preventing certain cofactors, namely thrombin and fibrin, from working correctly.
How effective are anticoagulants?
Warfarin and newer anticoagulants equally effective for long-term treatment of blood clots. Warfarin and newer anticoagulants work equally well to prevent blood clots in extended treatment after venous thromboembolism. One clot is prevented for every 15 people receiving either anticoagulant. Aspirin is ineffective.What is the mechanism of action of warfarin?
Warfarin competitively inhibits the vitamin K epoxide reductase complex 1 (VKORC1), which is an essential enzyme for activating the vitamin K available in the body. Through this mechanism, warfarin can deplete functional vitamin K reserves and therefore reduce the synthesis of active clotting factors.
Why do anticoagulants cause bleeding?A possible side effect of anticoagulants is excessive bleeding (haemorrhage), because these medicines increase the time it takes for blood clots to form. Some people also experience other side effects.
Article first time published onWhat is difference between antiplatelet and anticoagulant?
Anticoagulants such as heparin or warfarin (also called Coumadin) slow down your body’s process of making clots. Antiplatelet drugs, such as aspirin, prevent blood cells called platelets from clumping together to form a clot.
Why heparin is used as an anticoagulant?
Heparin is a naturally occurring anticoagulant that prevents the formation and extension of blood clots. Heparin does not break down clots that have already formed (unlike tissue plasminogen activator) but allows fibrinolysis to work normally to break down clots.
What is the difference between blood thinners and anticoagulants?
Anticoagulants, more commonly referred to as “blood thinners,” work by inhibiting the clotting factors. Antiplatelets work by inhibiting the enzymes that cause the platelets to clump together.
How is anticoagulant administered?
Anticoagulants are given either in oral form or by injection. Most injectable forms are administered in the hospital. The type of anticoagulant prescribed depends upon the condition being prevented.
When are anticoagulants contraindicated?
An oral anticoagulation contraindication was defined as the presence of one or more of the following: severe, chronic blood dyscrasia; intracranial mass; intracranial hemorrhage; severe/major gastrointestinal bleeding; and end-stage liver disease.
When does anticoagulant heparin start working?
Heparin rapidly reduces the ability of the blood to clot. Heparin works immediately following direct IV injection or infusion. Works within 20 to 60 minutes following deep SC injection.
How does Lovenox work?
Lovenox (enoxaparin) is an anticoagulant (blood thinner) that works by blocking the activity of certain blood-clotting proteins. As a result, blood clots are less likely to form in your legs, lungs, heart, or other blood vessels.
Where do anticoagulants work in the clotting cascade?
Anticoagulants derive their effect by acting at different sites of the coagulation cascade. Some act directly by enzyme inhibition, while others indirectly, by binding to antithrombin or by preventing their synthesis from the liver (vitamin K dependent factors).
How is Lovenox metabolized?
Enoxaparin and dalteparin are metabolized in the liver by desulfation and/or depolymerization to lower molecular weight fragments with reduced biologic activity.
What kind of anticoagulant is heparin?
Heparin is a prescription medicine used to treat and prevent the symptoms of blood clots caused by medical conditions or medical procedures. Heparin may be used alone or with other medications. Heparin belongs to a class of drugs called Anticoagulants, Cardiovascular, Anticoagulants, Hematologic.
What is the pharmacodynamics of warfarin?
Warfarin is essentially completely absorbed, reaching a maximum plasma concentration between 2 and 6 hours. It distributes into a small volume of distribution (10 L/70kg) and is eliminated by hepatic metabolism with a very small clearance (0.2 L/h/70kg). The elimination half-life is about 35 hours.
Why is heparin started before warfarin What is the mechanism of action of warfarin?
Because of the delay in factor II (prothrombin) suppression, heparin is administered concurrently for four to five days to prevent thrombus propagation. Loading doses of warfarin are not warranted and may result in bleeding complications.
How effective is warfarin in preventing clots?
The multi-center Prevention of Recurrent Venous Thromboembolism (PREVENT) trial found a 64 percent reduction in episodes of DVT and pulmonary embolism in study participants taking low-dose warfarin compared to those taking a placebo.
Is warfarin an oral anticoagulant?
In the last fifty years the warfarin has been considered the oral anticoagulant of choice. However, its use is limited by a narrow therapeutic index and by a complex pharmacodynamics, which requires regular adjustments and monitoring of the dose.
Is warfarin a direct oral anticoagulant?
Vitamin K antagonists, such as warfarin, have been the anticoagulants of choice for many years for patients with AF and other thrombotic conditions. The introduction of direct oral anticoagulants (DOACs) as alternatives represents a major advance in anticoagulation.
Do anticoagulants raise blood pressure?
The results demonstrate that warfarin therapy at conventional doses does not increase systolic blood pressure or pulse pressure in patients with diabetes and hypertension.
Why do blood thinners make you cold?
A blood thinner works by slowing or impairing the blood’s ability to clot, Dr. Andersen said, and will not make someone feel colder.
Can anticoagulants cause anemia?
(HealthDay News) — For patients with atrial fibrillation receiving anticoagulant treatment, the presence of anemia is associated with increased risk of thromboembolic events, bleeding complications, and mortality, according to research published online February 13 in the Journal of Thrombosis and Haemostasis. B.
When do you use anticoagulants and antiplatelets?
Anticoagulants and antiplatelets are medicines that reduce blood clotting in an artery, vein or the heart. Doctors prescribe these to help prevent heart attacks and strokes caused by blood clots. Blood clots can block blood flow to your heart or your brain causing a heart attack or stroke.
What is the primary mechanism of action of antiplatelet drugs?
Mechanism of action: Aspirin (acetylsalicylic acid) irreversibly inhibits prostaglandin H synthase (cyclooxygenase-1) in platelets and megakaryocytes, and thereby blocks the formation of thromboxane A2 (TXA2; a potent vasoconstrictor and platelet aggregant).
What is the main difference between an anticoagulant and a thrombolytic?
The anticoagulants prevent the formation of clots that inhibit circulation. The antiplatelets prevent platelet aggregation, clumping together of platelets to form a clot. The thrombolytics, appropriately called clot busters, attack and dissolve blood clots that have already formed.