What is fibrinolytic system

Lily Fisher
Published Feb 20, 2026
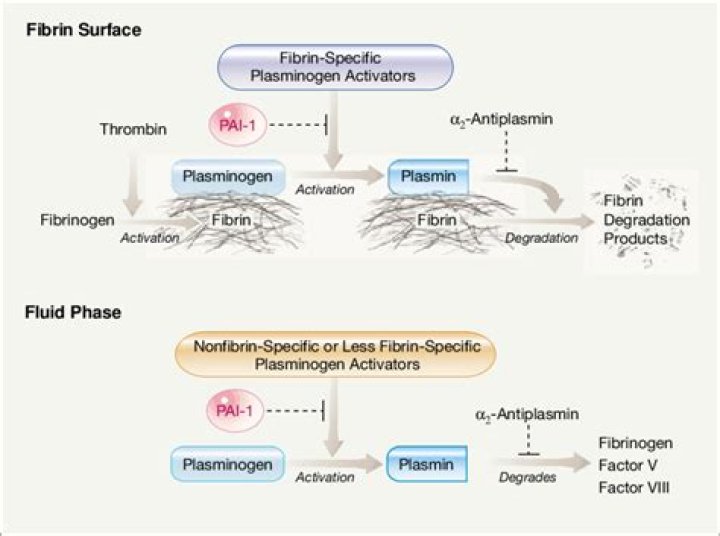
The fibrinolytic system functions to remove the clot after the vasculature is repaired, as well as to degrade clots that form in the bloodstream. The final step in this pathway is the plasmin-mediated cleavage of fibrin, creating fibrin degradation products.
What does the fibrinolytic system mean?
Fibrinolysis. The fibrinolytic system removes unwanted fibrin deposits to improve blood flow following thrombus formation, and to facilitate the healing process after injury and inflammation.
How do Fibrinolytics work?
Fibrinolytic drugs work by activating the so-called fibrinolytic pathway. This distinguishes them from the anticoagulant drugs (coumarin derivatives and heparin), which prevent the formation of blood clots by suppressing the synthesis or function of various clotting factors that are normally present in the blood.
What are Fibrinolytics give examples?
Thrombolysis refers to the dissolution of the thrombus due to various agents while fibrinolysis refers specifically to the agents causing fibrin breakdown in the clot. Antifibrinolytics, such as aminocaproic acid (ε-aminocaproic acid) and tranexamic acid are used as inhibitors of fibrinolysis.Which of the following is a fibrinolytic?
There are three major classes of fibrinolytic drugs: tissue plasminogen activators (tPAs), streptokinase, and urokinase. While drugs in these three classes all have the ability to effectively dissolve blood clots, they differ in their detailed mechanisms in ways that alter their selectivity for fibrin clots.
Is heparin fibrinolytic therapy?
Intravenous administration of heparin seems justified, specially if rtPA is used as fibrinolytic agent. Potent new drugs capable of inhibiting platelets an the coagulation cascade emerge as a promising future.
Are Fibrinolytics and thrombolytics the same?
Thrombolytic treatment is also known as fibrinolytic or thrombolysis to dissolve dangerous intravascular clots to prevent ischemic damage by improving blood flow.
Why do people need fibrinolytic drugs?
Fibrinolytics are used to disrupt clots that have formed in situations such as acute myocardial infarction, acute ischemic stroke, and massive pulmonary embolism.Is streptokinase a fibrinolytic?
Streptokinase is the least expensive fibrinolytic agent, but unfortunately, its antigenicity and its high incidence of untoward reactions limit its usefulness in the clinical setting.
What is fibrinolytic therapy for MI?Fibrinolytic therapy, also known as thrombolytic therapy, is used to lyse acute blood clots by activating plasminogen, resulting in the formation of plasmin, which cleaves the fibrin cross-links causing thrombus breakdown.
Article first time published onWhat are the major side effects of TPA?
- Pulmonary embolism.
- Cholesterol embolism.
- Abnormal heartbeats.
- Allergic reactions.
- Re-embolization of deep DVT venous thrombi during treatment of acute massive pulmonary embolism.
- Angioedema.
Which fibrinolytic is most effective and why?
Streptokinase is used much less frequently than other fibrinolytic drugs. The effectiveness of any fibrinolytic agent is greatest with fresh thrombus and if a large surface area of thrombus is exposed to the drug.
Why are Fibrinolytics not used in Nstemi?
In NSTEMI the blood flow is present but limited by stenosis. In NSTEMI, thrombolytics must be avoided as there is no clear benefit of their use. If the condition stays stable a cardiac stress test may be offered, and if needed subsequent revascularization will be carried out to restore a normal blood flow.
Is Urokinase is a fibrinolytic agent?
Urokinase is the fibrinolytic agent that is most familiar to interventional radiologists and that has been used most often for peripheral intravascular thrombus and occluded catheters. Urokinase is a physiologic thrombolytic agent that is produced in renal parenchymal cells.
When is fibrinolytic therapy indicated?
Fibrinolytic Therapy and ACS/AMI Fibrinolytic therapy may also be indicated if the signs and symptoms of a myocardial infarction last longer than 15 minutes and less than 12 hours and if PCI (percutaneous coronary intervention) is not available within 90 minutes of medical contact.
How do you pronounce Fibrinolytics?
noun, plural fi·bri·nol·y·ses [fahy-bruh-nol-uh-seez].
What is an absolute contraindication for the use of Fibrinolytics in a patient with a stemi?
Absolute contraindications for fibrinolytic use in STEMI include the following: Prior intracranial hemorrhage (ICH) Known structural cerebral vascular lesion. Known malignant intracranial neoplasm.
What is the most common complication of fibrinolytic therapy?
The most feared complication of fibrinolysis is intracranial hemorrhage (ICH), but serious hemorrhagic complications can occur from bleeding at any site in the body. Risk factors for hemorrhagic complications include the following: Increasing age. Lower body weight.
Why is heparin given during MI?
The roles of heparin and warfarin in reducing morbidity and mortality after acute myocardial infarction (AMI) are reviewed. Full-dose i.v. heparin, with or without thrombolytic therapy, is indicated for the prevention of reinfarction and thromboembolism after AMI.
Do you give aspirin before fibrinolytic therapy?
Furthermore, the beneficial effects of aspirin and clopidogrel as adjunctive therapy with fibrinolysis are well established and these agents should be given before or with the fibrinolytic. Aspirin should be administered immediately if not already taken by the patient at home or administered by EMS before arrival.
What is the meaning of plasmin?
Definition of plasmin : a proteolytic enzyme that dissolves the fibrin of blood clots.
Which drug is a pro drug of streptokinase?
Plasmin is produced in the blood to break down fibrin, the major constituent of blood thrombi, thereby dissolving clots once they have fulfilled their purpose of stopping bleeding. Extra production of plasmin caused by streptokinase breaks down unwanted blood clots, for example, in the lungs (pulmonary embolism).
How does alteplase differ from streptokinase?
Alteplase is a pharmacologic tPA and functions in the same way. Streptokinase: Streptococci produce this substance. When given as a drug, streptokinase works with the body’s own supply of plasminogen. Plasminogen, in the presence of streptokinase, will become plasmin at a fast rate.
Is Ischemic Stroke?
Ischemic stroke is one of three types of stroke. It’s also referred to as brain ischemia and cerebral ischemia. This type of stroke is caused by a blockage in an artery that supplies blood to the brain. The blockage reduces the blood flow and oxygen to the brain, leading to damage or death of brain cells.
Why can you only give tPA within 3 hours?
The timing of treatment is important, because giving a strong blood thinner like tPA during a stroke can cause bleeding inside the brain. The longer a patient waits to get treatment, the more likely it is that the risks of treatment will outweigh the benefits.
What is the role of Fibrinolytics in myocardial infarction and stroke?
The aim of fibrinolytics is to dissolve blood clots that can cause serious and potentially life-threatening damage if not removed in a timely manner. The mechanism of this benefit relates to maximizing tissue salvage by early restoration of blood flow and thereby enhancing both early and long-term survival.
What are the benefits of administering fibrinolytic therapy in the early management of stemi?
Improved left ventricular function and even more impressive improvements in survival rates have been demonstrated consistently in controlled studies. Benefit is related to the restoration of myocardial blood flow. Maximal benefit is achieved with early and sustained restoration of coronary artery patency.
Is tPA a fibrinolytic?
Tissue plasminogen activator (tPA) is a naturally occurring fibrinolytic agent found in vascular endothelial cells and is involved in the balance between thrombolysis and thrombogenesis.
Is tPA a blood thinner?
TPA treatment has risks. There is approximately a 3% chance of symptomatic bleeding (symptomotic hemorrhage) into the brain (because TPA thins the blood) compared to 0.2% if TPA is not given. If bleeding into the brain happens after TPA is given, it may cause your stroke symptoms to be worse and may result in death.
What drugs are used in thrombolytic therapy?
- Eminase (anistreplase)
- Retavase (reteplase)
- Streptase (streptokinase, kabikinase)
- t-PA (class of drugs that includes Activase)
- TNKase (tenecteplase)
- Abbokinase, Kinlytic (rokinase)
When is alteplase used?
Alteplase injection is used to dissolve blood clots that have formed in the blood vessels. It is used immediately after symptoms of a heart attack occur to improve patient survival. It is also used after symptoms of a stroke and to treat blood clots in the lungs (pulmonary embolism).