Which rib is thoracentesis

Andrew Campbell
Published Feb 21, 2026
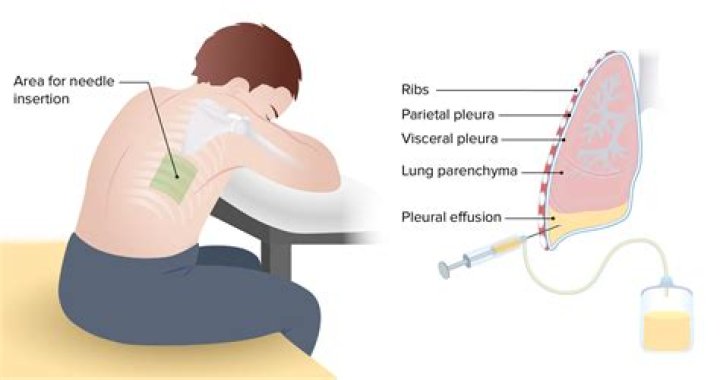
In order to minimize potential injury of the diaphragm, the lowest recommended level for thoracentesis is between the eighth and ninth ribs (eighth intercostals space). Mark the area of needle insertion by pressing a pen or pen cap firmly on the skin creating an indentation that will remain after the ink is washed off.
Where do you place the needle for thoracentesis?
Warnings and Common Errors for Thoracentesis Be sure to insert the thoracentesis needle just above the upper edge of the rib and not below the rib, to avoid the intercostal blood vessels and nerves at the lower edge of each rib.
Where do you put the needle for aspiration of pleural effusion?
Insert the needle along the upper border of the rib while aspirating and advance it into the effusion. When fluid or blood is aspirated, insert the catheter over the needle into the pleural space and withdraw the needle, leaving the catheter in the pleural space.
In which intercostal space is Thoracocentesis done?
Needle thoracocentesis is a life saving procedure, which involves placing a wide-bore cannula into the second intercostal space midclavicular line (2ICS MCL), just above the third rib, in order to decompress a tension pneumothorax, as per Advanced Trauma Life Support (ATLS) guidelines.What left thoracentesis?
Thoracentesis is a procedure to remove fluid or air from around the lungs. A needle is put through the chest wall into the pleural space. The pleural space is the thin gap between the pleura of the lung and of the inner chest wall. The pleura is a double layer of membranes that surrounds the lungs.
Is a thoracentesis a chest tube?
A pleurodesis procedure is usually performed through a chest tube placed at the time of the thoracentesis. A medication such as doxycycline is injected into the pleural space, which triggers an inflammatory reaction on the pleural membrane that lines the outside of the lung and the inside of the chest wall.
When do you use a chest tube vs thoracentesis?
The only indication for emergency needle thoracocentesis is a rapidly deteriorating patient who is developing a life-threatening tension pneumothorax. In contrast to thoracocentesis, chest tube insertion is frequently performed as an emergency procedure.
Where is 5th intercostal space?
The apex (the most inferior, anterior, and lateral part as the heart lies in situ) is located on the midclavicular line, in the fifth intercostal space. It is formed by the left ventricle. The base of the heart, the posterior part, is formed by both atria, but mainly the left.What is the difference between Thoracocentesis and thoracentesis?
Thoracocentesis, also known as thoracentesis or pleural tap, is an invasive procedure to remove fluid or air from the pleural space for diagnostic or therapeutic purposes. A cannula, or hollow needle, is carefully introduced into the thorax, generally after administration of local anesthesia.
How do you find the 5th intercostal space?Move down over the next 2 ribs and you have found the 4th intercostal space. Where this space meets the sternum is the position for V2. From this position, slide your fingers downward over the next rib and you are in the 5th intercostal space .
Article first time published onWhich intercostal space is used for pleural effusion?
Procedure-technique-equipment-position Some sources recommend the mid-axillary line in the 6th, 7th, or 8th intercostal space. It is critical that the patient hold his or her breath to avoid piercing of the lung. The pleural fluid collection is located and marked under real-time ultrasound guidance.
What is the most common site for the pleural aspiration?
The conventional site for aspiration is posteriorly, approximately 10 cm lateral to the spine (mid-scapular line) and 1-2 intercostal spaces below the upper level of the fluid.
Which of the following is a contraindication against performing thoracentesis?
Relative contraindications to diagnostic thoracentesis include a small volume of fluid (< 1 cm thickness on a lateral decubitus film), bleeding diathesis or systemic anticoagulation, mechanical ventilation, and cutaneous disease over the proposed puncture site.
What color should fluid drained from lungs be?
A thoracentesis is a procedure used to drain excess fluid from the space outside of the lungs but inside the chest cavity. Normally, this area contains about 20 milliliters of clear or yellow fluid. If there’s excess fluid in this area, it can cause symptoms such as shortness of breath and coughing.
What does the color of pleural effusion mean?
Pale yellow fluid may be associated with exudates; bloody fluid with malignancy, trauma, and pulmonary infarction; black with an Aspergillus infection; and dark green with bilothorax. The WBC and differential are also used to help determine the cause of a pleural effusion.
What is the difference between thoracentesis and pleural drainage?
Thoracentesis refers to the removal of fluid from the space between the lungs and the chest wall, called the pleural cavity. Paracentesis refers to removing fluid from the abdominal cavity.
In which edge of the ribs are performed needle puncture of the pleural cavity?
Needle insertion should target the upper edge of the rib in order to avoid injury to the neurovascular bundle which runs at the inferior margin of each rib.
What color should chest tube drainage be?
The first few days after your surgery, the fluid draining from your chest may be dark red. This is common. As you heal, it may look pink or pale yellow. If fluid is draining from your chest, it will flow through your chest tube and into your Pneumostat’s collection chamber.
What is the difference between Transudative and exudative fluid?
“Transudate” is fluid buildup caused by systemic conditions that alter the pressure in blood vessels, causing fluid to leave the vascular system. “Exudate” is fluid buildup caused by tissue leakage due to inflammation or local cellular damage.
What does a thoracentesis look for?
Thoracentesis uses imaging guidance and a needle to help diagnose and treat pleural effusions. This is a condition in which the space between the lungs and the inside of the chest wall contains excess fluid. Thoracentesis helps determine the cause of the excess fluid.
Who performs a thoracentesis?
The following specialists perform thoracentesis: Pulmonologists specialize in the medical care of people with breathing problems and diseases and conditions of the lungs. Pediatric pulmonologists specialize in the medical care of infants, children and adolescents with diseases and conditions of the lungs.
Where is a chest tube placed for a Hemothorax?
For hemothorax or pleural effusion, typically a straight tube is placed posterior and toward apex and/or a right-angled tube can be placed at the base of lung and diaphragm.
What is another name for thoracentesis?
Thoracentesis /ˌθɔːrəsɪnˈtiːsɪs/, also known as thoracocentesis (from Greek θώραξ thōrax ‘chest, thorax’—GEN thōrakos—and κέντησις kentēsis ‘pricking, puncture’), pleural tap, needle thoracostomy, or needle decompression (often used term) is an invasive medical procedure to remove fluid or air from the pleural space …
Why is chest radiography required pre and post thoracentesis?
Pneumothorax is the most common serious procedural complication and the principal reason to order postprocedural chest radiography. Less common complications include hemothorax, re-expansion pulmonary edema, infection, subdiaphragmatic organ puncture, and procedure-related death.
When should thoracentesis be done?
Thoracentesis should be performed diagnostically whenever the excessive fluid is of unknown etiology. It can be performed therapeutically when the volume of fluid is causing significant clinical symptoms. Typically, diagnostic thoracentesis is a small volume (single 20cc to 30cc syringe).
Where is the 4th and 5th intercostal space?
The location of the 4th and 5th intercostal space is related to the length of the sternum. It is 77% of the sternal length that measures 15 cm for the 4th intercostal space. The position of the V1 and V2 electrodes decreases to 57% when the sternal length is 26 cm.
How do you find the 6th intercostal space?
Locate the 6th intercostal space by counting parasternally from the clavicle or from the manubriosternal synchondrosis (→ 3.5). Follow the course of the intercostal space in a lateral direction and locate SP-21 on the axillary midline (note: the intercostal space laterally curves upward).
Which rib is closest to the heart?
The base of the heart is located at the level of the third costal cartilage, as seen in Figure 1. The inferior tip of the heart, the apex, lies just to the left of the sternum between the junction of the fourth and fifth ribs near their articulation with the costal cartilages.
Where is 4th intercostal space?
The location of the 4th and 5th intercostal space is related to the length of the sternum. It is 77% of the sternal length that measures 15cm for the 4th intercostal space. The position of the V1 and V2 electrodes decreases to 57% when the sternal length is 26cm.
Where is the 2nd rib located?
The second rib attaches to the sternum at the sternal angle. Since the first rib is hidden behind the clavicle, the second rib is the highest rib that can be identified by palpation. Thus, the sternal angle and second rib are important landmarks for the identification and counting of the lower ribs.
Where are the posterior ribs?
Posteriorly, the head of the rib articulates with the costal facets located on the bodies of thoracic vertebrae and the rib tubercle articulates with the facet located on the vertebral transverse process. The angle of the ribs forms the most posterior portion of the thoracic cage.